Open Access
Review
26 March 2026
Denture
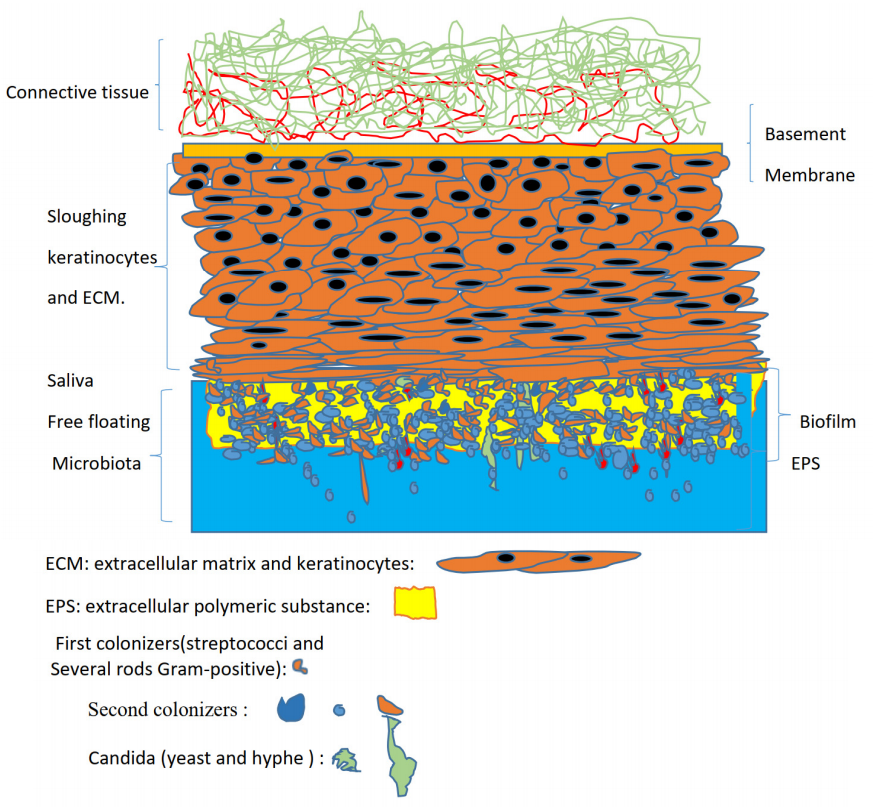
mycofilms (DMs) are complex, structured microbial communities that develop on
removable dental prostheses and shape the oral microbiota of denture wearers.
Up to three-quarters of individuals wearing removable dentures may develop
denture stomatitis (DS), a highly prevalent inflammatory condition of the oral
mucosa. Candida species are detected in approximately 70–80% of DS cases,
supporting the concept of DS as a denture-associated oral candidiasis. The
denture “mycofilm” is a polymicrobial network—dominated by bacterial and fungal
taxa—embedded in an extracellular matrix. In the absence of effective denture
hygiene, prostheses constitute a reservoir of microorganisms and may promote chronic or latent infection, particularly in
vulnerable patients. Metagenomic studies of denture-associated biofilms in DS
reveal a multi-kingdom community with strong bacterial–fungal
interrelationships. Reported eukaryotic genera include Candida (including
Nakaseomyces/Candida glabrata), Saccharomyces, and Malassezia, among others.
Because DMs are located at the interface between an abiotic surface (the denture)
and a biotic surface (the mucosa), they are exposed to repeated compressive and
shear forces during mastication. Their viscoelastic properties, together with
saliva-mediated viscosity, facilitate spreading, mechanical resilience, and
persistence. Despite
mechanical and chemical cleaning procedures, denture mycofilms may persist due
to their architecture, composition, and adaptive mechanical behavior. These
properties should be considered when designing preventive and therapeutic
strategies for denture stomatitis, while accounting for patient-related
systemic risk factors.utf-8
Pierre Le Bars*
Ayépa Alain Kouadio
Octave Nadile Bandiaky
Yves Amouriq
Fungal Res.
2026,
1
(1), 10001;
Open Access
Communication
20 May 2026
Blueberries
(Vaccinium corymbosum L.), valued for their nutritional benefits and
economic significance, have become Peru’s leading agro-export crop. However,
intensive cultivation can lead to phytosanitary problems if not addressed promptly,
posing a serious threat to blueberry production. This study aimed to isolate
and identify the causal agent of leaf spot symptoms initially observed in
blueberries cultivated in Peru, marking the first formal documentation of its
presence in the country. In 2022, leaf spot symptoms were recorded on V.
corymbosum cv. Biloxi, in the north of Lima, Peru. Field observations
revealed necrotic, sunken spots on leaves and fruits, with 4.84% of leaves
diseased and 1.28% of fruits affected. Pathogen isolation and microscopic
studies identified Alternaria alternata as the primary causal agent,
which was confirmed by genome sequencing using Oxford Nanopore Technology.
Pathogenicity tests demonstrated the fungus’ ability to reproduce symptoms
identical to those observed in the field, fulfilling Koch’s postulates. Under
experimental conditions, disease severity increased over time, with the
affected leaf area ranging from 9.35% to 25.61% between 7 and 14 days
post-inoculation. This study establishes A. alternata as a pathogen of
blueberries in Peru and provides essential insights for future research and
strategies to mitigate its impact on the industry.utf-8
Ricardo Velasquez
Valentina Osorio
Ana Maria Leiva
Juan Manuel Pardo
Alejandra Gil-Ordóñez
Ida Bartolini
Wilmer J. Cuellar*
Fungal Res.
2026,
1
(1), 10002;
 Open Access
Open Access