Associations of Oppositional Defiant Disorder, Irritability, and Headstrong Dimensions with Other Psychological Disorders in Adolescents
Received: 22 December 2025 Revised: 04 January 2026 Accepted: 04 February 2026 Published: 26 February 2026
© 2026 The authors. This is an open access article under the Creative Commons Attribution 4.0 International License (https://creativecommons.org/licenses/by/4.0/).
1. Introduction
Oppositional Defiant Disorder (ODD) refers to a pattern of behavioral responses related to oppositionality, vindictiveness, argumentativeness, and irritability that cause conflicts with adults and authority figures [Diagnostic and Statistical Manual-5 (DSM-5-TTR); American Psychiatric Association (APA), 2022]. In the DSM-5-TR, there are eight symptoms for ODD, grouped into three dimensions, namely anger/irritable mood (comprising temper, touchy, and angry symptoms), argumentative/defiant (comprising argues, defies, annoys, and blames others symptoms), and vindictiveness (comprising a single spiteful symptom). Factor analyses of these symptoms have generally supported two closely associated dimensions. They are an affective dimension (also referred to as irritability or negative affect) and a headstrong dimension (also referred to as behavioral or defiant; [1,2,3,4,5]), with the irritability and headstrong dimensions being more closely associated with internalizing and externalizing problems, syndromes and disorders, respectively (e.g., [2,5,6]. However, the vast majority of these studies examined internalizing and externalizing problems and syndromes, and not the specific disorders as presented in DSM-5 or earlier versions of the DSM. Most studies used observed and not latent scores. Additionally, although eating and neurodevelopmental disorders are also common in adolescents, their associations with the ODD irritability and headstrong dimensions have yet to be examined. Considering these omissions, the major aim of the current study was to examine how latent scores for the DSM-5 ODD dimensions were differentially and uniquely associated with a range of specific DSM-5 internalizing, externalizing, neurodevelopmental, and eating disorders in a group of clinic-referred adolescents.
1.1. ODD: Symptoms, Dimensions, and Associations with Internalizing and Externalizing Dimensions and Syndromes/Disorders
To date, many studies have examined the factor structure of the ODD symptoms. While various models have been proposed for ODD, differing in terms of number and names of the dimensions, and content in the dimensions (e.g., [1,2,4,5,6,7]), they all appear to have an affective dimension (also referred to as irritability or negative affect) and a headstrong dimension (also referred to as behavioral or defiant; e.g., [1,2,3,4,5]). Considering this, it has been proposed that these dimensions will have different etiologies [7] and are worthy of focus. To ensure the conceptual distinction and validity of these dimensions and to make our results clinically relevant to DSM-5, we modelled our irritability and headstrong dimensions based on DSM-5 dimensions of ODD. As mentioned previously, DSM suggests three dimensions: anger/irritable (comprising symptoms of temper tantrums, anger, and touchiness), argumentative/defiant behavior (comprising symptoms of arguing with adults, purposefully annoying others, disobedience, and blaming others for one’s own mistakes), and vindictiveness (comprising a single symptom for spiteful/vindictiveness). Consequently, the scores for symptoms of temper, blame, and touchy can be summed to provide a score for the ODD irritability dimension; and scores for symptoms of argue, defy, annoy, and blame can be summed to provide a score for headstrong [7]. These scores were used in the current study. The remaining symptom for “spiteful” is not clearly related to irritability or headstrong [8].
To date, many studies have shown that although these dimensions are closely associated with each other (e.g., [1,5]), the irritability dimension is generally more closely associated and predictive of internalizing problems such as depression and anxiety, whereas the headstrong dimension is generally more closely associated and predictive of externalizing problems like ADHD and conduct disorders [2,6,7]. Although these associations have several explanations [9], a dominant view is that they reflect primarily shared emotion dysregulation problems associated positively with the irritability dimension of ODD and internalizing disorders in general; and shared emotional control difficulties in the headstrong dimension of ODD, and externalizing disorders in general being associated positively [9,10].
There are also studies that have failed to replicate these differential associations [5,8,11,12]. Leadbeater and Homel [8] reported that both internalizing and conduct problems (an externalizing disorder) were associated with both irritability and headstrong. More recently, Klos et al. [11] reported that while both the irritability and headstrong ODD dimensions demonstrated significant correlations with both the externalizing (overall externalizing problems, aggressive behavior, and rule-breaking behavior) and internalizing (overall internalizing problems, withdrawn, somatic complaints) syndrome on the Achenbach’s Youth Self Report Form (YSR), they were both more strongly correlated with the externalizing problems scales than with the internalizing problems scales. These findings suggest that headstrong, more than irritability, is more closely associated with both internalizing and externalizing disorders. In a longitudinal study that examined these associations using latent regression analysis, Mikolajewski et al. [12] found that both the ODD dimensions predicted uniquely antisocial behavior (alcohol use disorder, cannabis use disorder, and adult antisocial behavior) and overall externalizing problems, and that the expected unique relationships between the irritable dimension and specific internalizing disorders (major depressive disorder, social phobia, specific phobia, and panic disorder) were not found. Thus, their findings suggest that while headstrong is more closely associated with both internalizing and externalizing disorders, irritability has no relation with internalizing (and externalizing disorders). Such inconsistent findings raise the need for more careful studies in this area.
Notwithstanding the inconsistency, most researchers generally accept that ODD irritability is associated positive with internalizing disorders and problems. Internalizing disorders include different anxiety and depression disorders [13]. Although there are several different types of anxiety and depression disorders, each with certain unique features, they are highly comorbid with each other [14], and a common feature of the all the different anxiety and depression disorders is irritability [7,15,16]. Considering this, it can be speculated that ODD irritability, more than ODD headstrong, will be associated positively with the different anxiety and depression disorders. It is also generally accepted that ODD headstrong is associated positively with externalizing disorders and problems. Externalizing disorders include ODD and CD [13], and they are highly comorbid with each other [14,17]. Considering this, it can be speculated that ODD headstrong more than ODD irritability will be associated positively with the different externalizing disorders.
1.2. Limitations in Existing Findings
In addition to the inconsistent findings, there are limitations in the existing data in this area. First, past findings are limited in terms of how the externalizing and internalizing disorders (i.e., depression, anxiety, behavior problems) were measured and scored in the studies. In brief, they used composite scores or broadband scales, and even when narrowband scales were used, they did not correspond to the specific symptoms listed for them in DSM-5. For example, ADHD was based on the attention scale in the CBCL/YRF, not the specific DSM-5 ADHD symptoms for this disorder (see [1], for example). In our view, establishing the relationship of the ODD dimensions with psychological disorders based on their respective DSM-5 symptoms would provide a more clinically and diagnostically meaningful and useful understanding of the relationships of the ODD dimensions with other disorders.
Second, apart from internalizing and externalizing disorders, neurodevelopmental disorders [18,19] and eating disorders [20,21,22] are also common among adolescents. Besides ADHD, DSM-5 includes intellectual developmental disorder, communication disorders, autism spectrum disorder, neurodevelopmental disorder, motor disorder, and specific learning disorders as neurodevelopmental disorders. Apart from ADHD, the associations for the ODD dimensions with the other neurodevelopmental disorders have not been examined in past studies. Considering existing findings that adolescents with neurodevelopmental disorders [23,24,25] and eating disorders [26,27] often experience co-occurring mental health issues that include both internalizing and externalizing psychological problems and disorders, it could be speculated that the ODD dimensions would provide clinically useful insights on the comorbidity of the neurodevelopmental disorders with not only the ODD dimensions, but also internalizing and externalizing disorders, in general.
Regarding neurodevelopmental disorders, data show shared aetiological factors. The HI dimension of ADHD shares phenotypic traits, like impulsivity, under-controlled behaviors with ODD, and there is also evidence for shared genetic factors between ADHD dimensions and ODD dimensions [28,29]. Considering this, it is conceivable that both the irritability and headstrong dimensions would be positively associated with the ADHD IA and HI dimensions. Relatedly, there is evidence that both the ODD dimensions are associated positively with both the ADHD dimensions [30]. In relation to ASD, the association with ODD may reflect shared underlying issues such as emotion regulation difficulties, sensory overload, and communication challenges. Data show that individuals with ASD generally experience sensory overload (i.e., brains being overwhelmed by too much sensory input), contributing to emotional regulation difficulties, which, in turn, lead to intense frustration, emotional outbursts, irritability, and low emotional control. In this respect, neuropsychological processes involved in autism, like resistance to change or sensory overload, can be expected to trigger headstrong symptoms like defiance and anger. Therefore, it is possible that both the irritability and headstrong ODD dimensions could be associated positively with ASD. Consistent with this speculation, there is evidence that ODD irritability is associated with internalising problems but not externalising problems; and ODD defiance is associated with externalising but not internalising problems [31].
In relation to learning difficulties, at present, data show that ODD, including the irritability and headstrong dimensions, are negatively correlated with better academic attainment [2]. However, considering that the ODD headstrong dimension is characterized by argumentativeness, rule-breaking, and defiance, it can be speculated that this could potentially disrupt the learning process and, through this, lead to poor school and academic adjustment and performance [32,33]. Thus, it can be speculated that the ODD dimension for headstrong more than irritability, could be associated positively with learning difficulties. Although at present there are data showing that ODD, including the irritability and headstrong dimensions, are correlated negatively with better academic attainment [2], there is also evidence that these associations are not unique. Overall, therefore, despite the theoretical possibility that the ODD dimension for headstrong and, to a lesser degree, irritability could be associated positively with learning difficulties, the empirical evidence, albeit limited, does not appear to indicate unique associations for either ODD irritability or ODD headstrong with academic performance.
In relation to eating disorders, there is limited evidence that both AN and BN are associated with ODD [34,35]. However, we were unable to find any study that examined differential associations between AN and BN and the ODD dimensions of irritability and headstrong. However, it is conceivable that these associations may involve shared underlying vulnerabilities, such as impulsivity with bulimia nervosa [36], and emotional dysregulation with bulimia nervosa [37,38,39]. Considering this, it can be speculated that ODD headstrong will be more associated with AN than BN, and ODD irritability will be more associated with BN than AN.
Third, virtually all studies in this area have used correlation and ordinary least squares multiple regression analyses (MRA) with observed scores for examining the relationships of the ODD dimensions with the outcome variables (other disorders). Observed scores comprise measurement error that can distort the relationship between variables. In contrast, as latent variables have their measurement error removed from them, the relationship between variables can be examined without this error problem. Consequently, using latent scores can provide a clearer, more accurate understanding of the unique associations between the ODD dimensions and other disorders. Relatedly, a widely used methodology that applies latent scores is latent regression analysis (LRA), which is a form of structural equation modeling.
Fourth, past studies in this area have not considered the possibility of suppression effects when examining the relationships of the ODD dimensions with other disorders. Suppressor effects occur when the addition of a variable to a regression equation improves the prediction of another variable in the model. Suppression effects are highly relevant in this area of research as there is evidence that in instances where the predictors are highly correlated, as is the case between irritability and headstrong [1,5], suppressor effects are more likely [40]. Statistically, a suppression effect is interpreted when the association between a predictor variable and an outcome is increased in the regression model by the presence of another predictor. This increase is explained in terms of the other predictor removing irrelevant or extraneous variance from the original predictor [41]. In this context, the other variable is referred to as the suppressor, with the original predictor being the suppressed predictor. The suppression effect therefore, reveals the true relationship between the original predictor and the outcome. Both MRA with observed scores and LRA with latent scores can examine suppression effects. However, as the error variance in observed scores can distort findings, examining suppression using LRA with latent scores is preferred [42]. Therefore, in the context of the current study, examination of suppression effects, especially with LRA can provide a more nuance understanding of how the irritability and headstrong dimensions predict the dimensions for outcome disorders, including evidence of the interdependence of the ODD dimensions in the predictions of other disorders.
Overall, therefore, more studies are needed, covering not only internalizing and externalizing disorders, but also neurodevelopmental disorders and eating disorders as reflected in DSM-5. Using LRA with latent scores would be useful as they could have the potential to reveal a better understanding of the associations of the ODD dimensions with other disorders than correlation analysis and multiple regression analysis with observed scores. Additionally, examination of suppression effects for these relations using a latent score would further enhance this understanding.
1.3. Study Aims and Predictions
Given the inconsistency and limitation in existing findings in this area, the major aim of the current study was to use latent regression analysis (LRA) to examine unique associations of DSM-5 ODD irritability and headstrong dimensions with 14 common DSM-5 internalizing, externalizing, neurodevelopmental, and eating disorders. These were examined in a group of clinic-referred adolescents, a group known to have high comorbidity rates [43]. To compare the findings in the current study using LRA with the findings in past studies using correlation analysis and MRA with observed scores, we also examined these associations using simple regression analysis (SRA) and MRA. Using SRA instead of correlation analysis is acceptable, as the correlation coefficient and standardized beta coefficient in SRA are equivalent for the same pairs of variables. Additionally, suppression effects were examined in both the LRA and the MRA.
The disorders examined included several internalizing disorders [Generalized Anxiety Disorder (GAD), Persistent Depressive Disorder (PDD), Separation Anxiety Disorder (SAD), Obsessive-Compulsive Disorder (OCD), Posttraumatic Stress Disorder (PTSD)], eating disorders [Anorexia Nervosa (AN), and Bulimia Nervosa (BN)]; externalizing disorders [ADHD Predominantly Inattentive Presentation (ADHDIA), ADHD Predominantly Hyperactive-Impulsive Presentation (ADHDHI), Conduct Disorder (CD)], and neurodevelopmental disorders [Specific Learning Disorder with impairment in Reading (SLDR), Autism Spectrum Disorder (ASD), Language Disorder (LD), Speech Sound Disorder (SSD)]. Although ADHDHI and ADHDIA are considered neurodevelopmental disorders [13], we have viewed them here as externalizing disorders to keep in line with how they have been seen in past studies in this area. The scores for all disorders examined were obtained from the relevant items (corresponding to DSM-5 symptoms) in the Child and Adolescent PsychProfiler (CAPP-PRF [44]), a widely used measure in Australia to facilitate clinical diagnosis.
Notwithstanding the inconsistencies and limitations in the scores and analytical methods used in past studies, and based on what experts generally believe, we predicted that for both the MRA and the LRA, the irritability dimension would be associated more (potentially uniquely) with internalizing disorders, whereas the headstrong dimension would be associated more (potentially uniquely) with the externalizing disorders. Relatedly, we speculated that both the irritability and headstrong dimensions would be associated positively with ADHDIA and ADHDHI dimensions. In relation to ASD, we speculated that both the irritability and headstrong ODD dimensions could be associated positively with ASD. In relation to learning difficulties, it was speculated that the ODD dimension of headstrong, rather than irritability, would be positively associated with learning difficulties. In relation to eating disorders, it was speculated that ODD headstrong would be associated with bulimia nervosa, whereas ODD irritability would be with binge eating.
2. Method
2.1. Participants
There were no selection criteria restricting participation in the study. The initial sample comprised 951 adolescents. There were 376 (39.54%) females and 575 (60.46%) males. The mean age for all participants (N = 951) was 14.56 years (SD = 1.67 years; range = 11 to 17 years). A power analysis using the software provided by Soper (2026) for a medium effect size (0.15), with statistical power of 0.80, at p value 0.05 for two and three predictors (number of predictors in our regression models) indicated minimum sample sizes of 67 and 76, respectively. Thus, our sample was more than sufficient for the regression analyses.
For the LRA, we used full information maximum likelihood to deal with missing values, and therefore all the 951 participants were involved in this analysis [45]. However, missing values were considered for the SRA and MRA, and of the 951 participants, 90 participants or 9.46% had one or more missing values for the disorders. Additional analyses indicated that data were missing at random, and no missing value pattern for each of the variables was evident; there was also no evidence of monotonicity. Considering this, we removed participants with missing values for the SRA and MRA. This meant that the frequencies of missing values differed across the different disorders, and therefore the final sample examined in the SRA and MRA varied from disorder to disorder (see Table 1).
Table 1. Descriptives and Frequencies Meeting Symptom Threshold Number.
|
Disorder |
N |
Mean |
SD |
≥Threshold (%) |
|
|---|---|---|---|---|---|
|
Generalized Anxiety Disorder (GAD) |
944 |
17.80 |
7.92 |
285 (30.0) |
5 |
|
Separation Anxiety Disorder (SAD) |
923 |
7.47 |
8.07 |
131 (13.8) |
9 |
|
Persistent Depression Disorder (PDD) |
945 |
18.13 |
8.65 |
389 (40.9) |
2 |
|
Obsessive-Compulsive Disorder (OCD) |
916 |
6.82 |
6.25 |
38 (4.0) |
15 |
|
Posttraumatic Stress Disorder (PTSD) |
930 |
11.03 |
8.81 |
218 (22.9) |
7 |
|
Conduct Disorder (CD) |
935 |
6.89 |
7.99 |
290 (30.5) |
4 |
|
Attention-Deficit/Hyperactivity Disorder Predominantly Hyperactive-Impulsive Presentation (ADHDHI) |
944 |
14.60 |
9.89 |
125 (13.1) |
10 |
|
Attention-Deficit/Hyperactivity Disorder Predominantly Inattentive Presentation (ADHDIA) |
946 |
25.40 |
10.71 |
412 (43.3) |
1 |
|
Autism Spectrum Disorder (ASD) |
944 |
16.98 |
11.96 |
135(14.2) |
8 |
|
Specific Learning Disorder-Reading (SLDR) |
941 |
7.32 |
6.09 |
238 (25.0) |
6 |
|
Language Disorder (LD) |
944 |
13.76 |
9.55 |
106 (11.1) |
11 |
|
Speech Sound Disorder (SSD) |
921 |
3.38 |
4.47 |
106 (11.1) |
11 |
|
Bulimia Nervosa (BN) |
939 |
5.10 |
4.85 |
71 (7.5) |
13 |
|
Anorexia Nervosa (AN) |
923 |
3.73 |
5.08 |
71 (7.5) |
13 |
|
Oppositional Defiant Disorder (ODD) |
940 |
14.86 |
9.04 |
316 (33.2) |
3 |
|
ODD—Irritability |
944 |
6.76 |
4.07 |
- |
|
|
ODD—Headstrong |
941 |
8.06 |
5.35 |
- |
|
|
Valid N (listwise) |
861 |
||||
All parents and their adolescents in the study were recruited from a psychology clinic in Perth, the capital city of Western Australia. Table 1 shows for the different disorders, the frequencies of participants involved in the analyses, their mean and standard deviation scores, and the frequencies of individuals meeting the DSM-5 diagnostic symptom threshold numbers, and the rank order of these frequencies. As shown, the frequencies for the different disorders varied widely, with ADHDIA being most frequent (412 or 43.3%), and OCD having the lowest frequency (38 or 4%). The frequency for ODD was also high (316 or 33.2%).
Supplementary Table S1 shows the mean scores (SD) for the 7 ODD symptoms used in the study for all participants. The score for vindictive behavior (the remaining ODD symptoms) is not shown as it was not part of either the ODD headstrong or irritability dimension. As shown in the table, the mean scores for all participants together ranged from 1.62 to 2.48. The range for all 7 symptoms was 0 to 5. This can be interpreted to mean that there was limited evidence of range constraint for all symptoms rated.
Supplementary Table S2 shows the frequencies of comorbidity for the sample involved in the study. As shown, 20.2% of the individuals did not meet the symptom threshold for any disorder, and 16.4% met the symptom threshold for one disorder. The remaining 63.4% met the symptom threshold for two or more disorders. Overall, the mean number of comorbidities was 3.31 (SD = 2.97), and the medium number was 2. Thus, the sample can be considered to have relatively high comorbidity. Considering this, the sample examined can be considered reflective of a typical clinic group.
2.2. Measures
The parent-report form of the Child and Adolescent PsychProfiler (CAPP-PRF [44]) was used for quick screening of the 14 common DSM-5 disorders in children and adolescents, based on parent ratings. A unique feature of this measure is that the items in the different screening scales correspond to the DSM-5 disorder symptoms with the same name. Thus, there is close alignment between the items in the CAPP-PRF screening scales and DSM-5 diagnostic symptoms with the same names. A recent study employing the CAPP-PRF with adolescents supported the factor structure of the CAPP-PRF, with virtually all of the factor scales showing acceptable reliability (alpha and omega coefficients), and discriminant and concurrent validity, thereby demonstrating the utility of the CAPP-PRF screening scales for measuring the equivalent DSM-5 disorders in adolescents [44].
The CAPP-PRF has 126 items, with scales for the following disorders included in the study: Attention-Deficit/Hyperactive Disorder Predominantly Inattentive Presentation (ADHDIA), Attention-Deficit/Hyperactive Disorder Predominantly Hyperactive–Impulsive Presentation (ADHDHI), Oppositional Defiant Disorder (ODD), Conduct Disorder (CD), Specific Learning Disorder-Reading (SLDR), Autism Spectrum Disorder (ASD), Language Disorder (LD), Speech Sound Disorder (SSD), Generalized Anxiety Disorder (GAD), Persistent Depressive Disorder (PDD), Separation Anxiety Disorder (SAD), Obsessive-Compulsive Disorder (OCD), Posttraumatic Stress Disorder (PTSD), Anorexia Nervosa (AN), and Bulimia Nervosa (BN).
Each item in the CAPP-PRF is rated on a six-point Likert scale (never = 0, rarely = 1, sometimes = 2, regularly = 3, often = 4, and very often = 5). The total item scores for the different scales provided the scores for the different disorders. These scores were used in the simple and multiple regression analyses in this study. The scores for the ODD irritability and headstrong dimensions were computed using the CAPP-PRF ODD scale. As mentioned earlier, based on DSM-5 ODD diagnostic criteria, the ODD irritability dimension was based on the total scores for the temper, touchy, and angry items, and the headstrong dimension was based on the total scores for the argues, defies, annoys, and blames items. The inter-consistency reliability McDonald omega values for irritability and headstrong were 0.86 (95% CI = 0.85/0.87) and 0.87 (95% CI = 0.86/0.88), respectively.
For screening the different disorders, the item scores were recoded as follows: never, rarely, sometimes = 0; and regularly, often, and very often = 1. Although there are some exceptions to these scoring rules (e.g., for example, for conduct disorder symptoms, fighting with a weapon, and stealing were considered to be of sufficient severity that “sometimes” was scored as 1), the total recoded scores of items for each scale were used for screening the risk/possibility of the relevant disorder. These cut-off scores for each scale corresponded with the symptom threshold cut-off scores for them in the DSM-5. When the total recoded screening score for a scale was at or exceeded the screening cut-off score, the disorder that it corresponded to was considered to be at risk (e.g., if the cut-off screening score for the CAPP ODD scale was 4 or more, as the symptom threshold cut-off score for ODD in the DSM-5 is 4). Given the close alignment between the items in the CAPP screening scales and the symptoms of the corresponding DSM-5 disorders, this practice seems intuitively prudent for identifying adolescents at risk for these disorders.
2.3. Procedure
The CAPP-PRF has a designated website that is used for online screening of DSM-5 disorders. The parents of adolescents involved in the study provided ratings for the CAPP-PRF through this website. They were mostly referred by their psychologists, psychiatrists, pediatricians, general practitioners, or school. On completion of the CAPP-PRF, respondents were requested, if they so wished, to click on a statement consenting to their ratings being used for future research and instrument validation purposes. Only the CAPP-PRF ratings of parents and adolescents with consent were included in the current study.
2.4. Statistical Analysis
To test the independent associations between the ODD dimensions and the disorders, the disorder in question was regressed on the two ODD dimensions separately. SRA was used for observed scores, and LRA was used for latent scores. To test the unique associations between the ODD dimensions and the disorders, the disorder in question was regressed on the two ODD dimensions jointly. MRA was used for observed scores, and a more complex LRA model was used for latent scores. Gender was included as a covariate as it has shown differential associations with psychological disorders during adolescence [46,47,48]. These analyses would therefore reveal the unique associations of each ODD dimension (association for ODD irritability, controlling for headstrong and gender, and association for headstrong, controlling for irritability and gender) with the relevant disorder. Significant path coefficients between predictors and outcome variables indicate unique associations. Supplementary Figure S1 shows a schematic diagram illustrating the SEM model used to examine the unique associations of ADHDIA with the ODD dimensions. As mentioned earlier, the indicators for these latent factor scores were obtained from the relevant items (corresponding to the DSM-5 symptoms) in the CAPP-PRF [44]. We used SPSS Version 29 to conduct the simple and multiple regression analysis, and Mplus Version 7 [49] with maximum likelihood for the LRA. For both cases, we inferred the effect sizes of the coefficients using Cohen’s [50]) guidelines: r = 0.10, 0.30, and 0.50 correspond to small, medium, and large effect sizes, respectively.
Statistically, a suppression effect, whether examined using MRA or LRA, is interpreted when the association between a predictor variable (say A) and an outcome (say C) is increased in the regression model by the presence of another predictor (say B). This usually involves comparing the standardized beta value of the predictor in question (A) when examined jointly with the other predictor (B) with its standardized beta value when examined alone [51]. An added consequence of this is that in the regression analysis with both A and B as predictors, the standardized beta value of the other variable B, will show a stronger relationship (often with an opposite sign) with the outcome C compared to its standardized beta value when examined alone.
In this study, suppression was inferred when one of the predictors had a zero or a close to standardized beta coefficient with the outcome variable. However, it improved the overall prediction of the outcome (i.e., classic suppression), or when a variable that had a positive standardized beta coefficient with an outcome showed a negative standardized beta coefficient (i.e., negative suppression), or when both the predictors were related positively to the outcome, but negatively to each other (i.e., reciprocal suppression [52]).
3. Results
3.1. Findings Based on Observed Scores
Preliminary Analyses
Testing Assumptions for Multiple Regression Analysis. Prior to the regression analysis, we tested the assumptions for multiple regression analysis. First, we tested for the assumption that the relationships between the IVs and the DVs were liner by examining the scatterplots of the relationship between each of the IVs and the DVs. Second, we tested for the absence of multicollinearity in our data set by using the collinearity diagnostics option in SPSS. Third, we examined that the residuals were independent, using the Durbin-Watson statistic. Fourth, we tested for homoscedasticity, or the assumption that the variation in the residuals is similar at each point across the model, using the SPSS option, i.e., examining the plot of the standardized values predicted in each model against the standardized residuals obtained in the relevant models. Fifth, we examined whether the residuals were normally distributed using a normal probability plot. Sixth, we tested for outliers in terms of Cook’s Distance. Although details are not presented here because they involved an overwhelming volume of information that makes presentation and processing difficult (even as supplementary documents) in most instances, we found that assumptions were not violated.
Fit for the ODD model with Irritability and Headstrong Latent Factors. The fit values for the 2-factor oblique CFA model with ODD irritability and headstrong latent factors, examined using WLSMV estimation, were as follows: WLSMVχ2 =20.851, df = 13, p = 0.031; root mean square error of approximation (RMSEA) = 0.034 (90% CI = 0.015–0.052); comparative fit index (CFI) = 0.997; and Tucker-Lewis Index (TLI) = 0.995. Thus, based on guidelines proposed by Hu and Bentler [53] for evaluating model fit (RMSEA values close to 0.06 or below = good fit; CFI and TLI, values close to 0.95 or above = good fit), our 2-factor model showed good fit.
3.2. Independent Associations of the ODD Dimensions with Other Disorders Based on the Simple Regression Analyses
Table 2 shows the standardized beta coefficients of the ODD irritability and headstrong dimensions with the 14 disorders examined in the current study. Column 2 shows these for the MRA with both the ODD dimensions as predictors, and columns 3 and 4 show these for the SRA with irritability and headstrong, respectively, as predictors. As shown in this table, for the SRA, all 14 disorders examined in the study were associated positively with both irritability and headstrong. Except for SAD, all standardized beta involving the other internalizing disorders (GAD, PDD, OCD, and PTSD) with irritability were of strong effect sizes. The effect size for SAD was medium. Except for SAD and OCD, the standardized beta coefficients with headstrong were of medium effect sizes. These were small effect sizes for SAD and OCD. The standardized beta coefficients involving the externalizing disorders (CD, ADHDHI, and ADHDIA) with headstrong were of strong effect sizes. Except for ADHDIA, the standardized beta coefficients for CD and ADHDHI with irritability were also of strong effect sizes. For ADHDIA, this was of medium effect size. Except for ASD, all the standardized beta coefficients involving the neurodevelopmental disorders with both irritability and headstrong were of small effect sizes. ASD had a large effect size standardized beta coefficient with irritability, and a medium effect size standardized beta coefficient with headstrong. BN had a medium effect size standardized beta coefficient with irritability and a small effect size standardized beta coefficient with headstrong. BN had small effect sizes, standardized beta coefficients, for both irritability and headstrong.
Table 2. Standardized Patha Coefficients for ODD Dimensions with the Different Disorders for Multiple Regression Analysis and SEM Models with Irritability (I) alone, Headstrong (H) alone, and Irritability and Headstrong Together as Predictors.
|
Multiple Regression Analysis |
Structural Equation Modeling |
|||||
|---|---|---|---|---|---|---|
|
Predictors |
I & H Together |
I Alone |
H Alone |
I & H Together |
I Alone |
H Alone |
|
GAD |
||||||
|
Gender |
−0.13 ** |
−0.17 *** |
−0.17 *** |
−0.19 ** |
−0.30 *** |
−0.57 *** |
|
Irritability |
0.65 *** |
0.62 *** |
0.89 *** |
0.65 *** |
||
|
Headstrong |
−0.05 |
0.49 *** |
−0.29 *** |
0.44 *** |
||
|
SAD |
||||||
|
Gender |
−0.11 *** |
−0.13 *** |
−0.13 *** |
−0.14 * |
−0.21 *** |
0.08 ** |
|
Irritability |
0.33 *** |
0.30 *** |
0.36 *** |
0.23 *** |
||
|
Headstrong |
0.04 |
0.24 *** |
−0.16 * |
0.14 *** |
||
|
PDD |
||||||
|
Gender |
−0.11 *** |
−0.15 *** |
−0.15 *** |
−0.15 |
−0.26 *** |
−0.28 *** |
|
Irritability |
0.62 *** |
0.64 *** |
0.98 *** |
0.75 *** |
||
|
Headstrong |
0.02 |
0.53 *** |
−0.29 ** |
0.48 *** |
||
|
OCD |
||||||
|
Gender |
−0.09 ** |
−0.12 ** |
−0.12 ** |
−0.30 ** |
−0.48 *** |
−0.65 *** |
|
Irritability |
0.46 *** |
0.44 *** |
0.87 *** |
0.52 *** |
||
|
Headstrong |
−0.02 |
0.36 *** |
−0.41 ** |
0.32 *** |
||
|
PTSD |
||||||
|
Gender |
−0.12 *** |
−0.15 *** |
−0.15 *** |
−0.21 ** |
−0.31 *** |
−0.49 *** |
|
Irritability |
0.53 *** |
0.52 *** |
0.69 *** |
0.48 *** |
||
|
Headstrong |
−0.02 |
0.42 *** |
−0.26 ** |
0.32 *** |
||
|
CD |
||||||
|
Gender |
0.02 |
0.05 |
0.05 |
0.01 |
−0.09 ** |
−0.05 |
|
Irritability |
0.15 *** |
0.65 *** |
0.13 *** |
0.29 *** |
||
|
Headstrong |
0.59 *** |
0.72 *** |
0.18 *** |
0.29 *** |
||
|
ADHDHI |
||||||
|
Gender |
0.11 *** |
0.15 *** |
0.15 *** |
0.11 |
0.40 *** |
0.13 * |
|
Irritability |
−0.02 |
0.51 *** |
−0.06 |
0.51 *** |
||
|
Headstrong |
0.63 *** |
0.62 *** |
0.61 *** |
0.56 *** |
||
|
ADHDIA |
||||||
|
Gender |
0.15 *** |
0.18 *** |
0.18 *** |
0.20 * |
0.53 *** |
0.29 * |
|
Irritability |
−0.07 |
0.41 *** |
−0.23 * |
0.48 *** |
||
|
Headstrong |
0.56 *** |
0.52 *** |
0.76 *** |
0.57 *** |
||
|
ASD |
||||||
|
Gender |
0.05 |
0.04 |
0.04 |
0.16 |
0.20 * |
−0.06 |
|
Irritability |
0.40 *** |
0.54 *** |
0.55 *** |
0.64 *** |
||
|
Headstrong |
0.17 ** |
0.51 *** |
0.06 |
0.52 *** |
||
|
SLDR |
||||||
|
Gender |
0.06 |
0.07 * |
0.07 * |
0.07 |
0.25 * |
0.17 |
|
Irritability |
−0.09 |
0.08 * |
−0.26 |
0.11 * |
||
|
Headstrong |
0.19 ** |
0.13 *** |
0.40 ** |
0.18 *** |
||
|
LD |
||||||
|
Gender |
0.06 |
0.08 * |
0.08 |
0.06 |
0.15 * |
0.05 |
|
Irritability |
0.02 |
0.24 *** |
0.02 |
0.21 *** |
||
|
Headstrong |
0.22 *** |
0.28 *** |
0.01 |
0.21 *** |
||
|
SSD |
||||||
|
Gender |
0.00 |
0.01 |
0.01 |
0.03 |
0.06 |
−0.01 |
|
Irritability |
−0.07 |
0.15 *** |
0.09 |
0.15 *** |
||
|
Headstrong |
0.11 |
0.17 *** |
0.05 |
0.13 *** |
||
|
BN |
||||||
|
Gender |
−0.14 *** |
−0.14 *** |
−0.14 *** |
−0.22 *** |
−0.24 *** |
−0.31 |
|
Irritability |
0.27 *** |
0.39 *** |
0.23 *** |
0.19 *** |
||
|
Headstrong |
0.13 * |
0.35 *** |
−0.06 |
0.13 *** |
||
|
AN |
||||||
|
Gender |
−0.22 *** |
−0.24 *** |
−0.24 *** |
−0.26 *** |
−0.32 *** |
−0.38 |
|
Irritability |
0.33 *** |
0.30 *** |
0.30 *** |
0.18 *** |
||
|
Headstrong |
−0.04 |
0.22 *** |
−0.14 * |
0.11 *** |
||
Note. GAD = Generalized Anxiety Disorder; SAD = Separation Anxiety Disorder (SAD); PDD = Persistent Depressive Disorder; OCD = Obsessive-Compulsive Disorder; PTSD = Posttraumatic Stress Disorder; ADHDHI = Attention Deficit/Hyperactivity Disorder Predominantly Hyperactive-Impulsive Presentation; ADHDIA = Attention Deficit/Hyperactivity Disorder Predominantly Inattentive Presentation; CD = Conduct Disorder; ASD = Autism Spectrum Disorder (ASD); SLDR = Specific Learning Disorder with impairment in Reading; LD = Language Disorder; SSD = Speech Sound Disorder; BN = Bulimia Nervosa; AN = Anorexia Nervosa.* Significance at 0.05; ** significance at 0.01; *** significance at 0.001.
3.3. Unique Associations of the ODD Dimensions with Other Disorders Based on the Multiple Regression Analyses
As shown in column 2 of Table 2, the results of the MRA that examined the unique associations of irritability and headstrong with the psychological disorders showed that with the exception of SAD, all standardized beta values involving the other internalizing disorders (GAD, PDD, OCD, and PTSD) with irritability were of positive, strong effect sizes. It was of a positive medium effect size for SAD. The standardized beta values for all the internalizing disorders with headstrong were not significant. The standardized beta values involving all the externalizing disorders (CD, ADHDHI, and ADHDIA) with headstrong were all positive and of large effect sizes. The association with irritability was positive, and of low effect size with CD, but not significant for ADHDIA and ADHDHI. Except for ASD, all the standardized beta values involving the other neurodevelopmental disorders (SLDR, LD, and SSD) with irritability were not significant. These were of low effect size for SLDR and LD, and not significant for SSD with headstrong. The standardized beta values for ASD with irritability were of a positive strong effect size. The standardized beta values for ASD with headstrong were positive and of a small effect size. For both eating disorders, irritability was associated positively with a small effect size with irritability, and AN was associated positively with a medium effect size with irritability. The associations with headstrong were positive and of small effect size for BN, and not significant for AN.
3.4. Suppression Effects Based on the Multiple Regression Analyses
Comparing the standardized beta coefficients for the predictions of the outcomes when both the ODD dimensions were entered as predictors to their standardized beta coefficients. When each of the ODD dimensions was examined separately, it was indicated that for a number of disorders (GAD, OCD, PTSD, ADHDHI, ADHDIA, SLDR, and AN), one of the ODD dimensions that had a positive standardized beta coefficient when examined alone showed a negative standardized beta coefficient, and the other ODD dimension showing a stronger predictive effect when examined together. Although this is suggestive of negative suppression, we have not interpreted these as such because the absolute differences in the increase in standardized beta coefficients for the suppressed ODD dimensions were very small, mostly around 0.01 (ranging from 0.01 to 0.04).
4. Findings Based on Latent Scores
4.1. Latent Regression Analysis of the ODD Dimensions Separately with the Other Disorders
Table 2, Columns 6 and 7 show the standardized beta coefficients for the ODD irritability and headstrong dimensions with the 14 disorders examined in the LRA when the ODD dimensions were examined separately. As shown, except for SAD, all the other internalizing disorders (GAD, PDD, OCD, and PTSD) showed positive associations of medium or large effect sizes with both irritability and headstrong. SAD showed positive associations of small effect sizes with irritability and headstrong. Among the externalizing disorders, ADHDIA and ADHDHI showed positive associations of medium or large effect sizes with both irritability and headstrong. CD showed positive associations of small effect sizes with both irritability and headstrong. ASD showed positive associations of large effect sizes with both irritability and headstrong. For all the other neurodevelopmental disorders (SLDR, LD, and SSD), there were positive associations of small effect sizes with both irritability and headstrong. Both BN and AN showed small positive associations with irritability and headstrong.
4.2. Unique Associations and Suppression Effects for the of the Associations of ODD Dimensions with the Other Disorders Based on LRA
Table 2, Column 5 shows the standardized beta coefficients for the ODD irritability and headstrong dimensions with the 14 disorders examined in the LRA when the ODD dimensions were examined jointly. As shown, GAD, PDD, OCD, and PTSD were associated positively with large effect sizes with irritability, and OCD was associated positively with a medium effect size with irritability. Thus, there was evidence of unique positive associations of large or medium effect sizes for all the internalizing disorders with irritability. In contrast, GAD, SAD, PDD, and PTSD were associated negatively with low effect sizes with headstrong, and OCD was associated negatively with medium effect sizes with headstrong. Seen together with their standardized beta coefficients for the ODD dimensions when they were examined separately, the findings for the associations involving headstrong are better interpreted as having suppression effects on the relations between irritability and the internalizing disorders (thereby increasing the strength of these associations) than unique negative associations between headstrong and the internalizing disorders.
Among the externalizing disorders, ADHDIA and ADHDHI were associated positively with a large effect size with headstrong. HI showed no association with irritability, whereas ADHDIA showed a negative association of small effect size with irritability. CD was associated positively with a small effect size with both irritability and headstrong. Thus, there was evidence of a unique positive association of large effect size for ADHDIA and ADHDHI with headstrong, and a unique positive association of small effect size for CD with irritability and headstrong. Seen together with their standardized beta coefficients for the ODD dimensions when they were examined separately, the findings for the associations involving irritability and ADHDIA are better interpreted as irritability having a suppression effect on the relations between headstrong and ADHDIA (thereby increasing the strength of this association) than unique negative associations between irritability and ADHDIA.
ASD was associated positively with a large effect size with irritability, and it was not associated with headstrong. LD and SSD showed no associations with both irritability and headstrong. SLDR showed positive associations of medium effect size with headstrong and a negative association of low effect size with irritability. Thus, there was evidence of a unique positive association of large effect size between ASD with irritability, and a unique positive association of medium effect size for SLDR with headstrong. Seen together with their standardized beta coefficients for the ODD dimensions when they were examined separately, the findings for the negative association involving irritability and SLDR are better interpreted as irritability having a suppression effect on the relation between headstrong and SLDR (thereby increasing the strength of this association) than unique negative associations between irritability and SLDR.
BN and AN were associated positively with small and medium effect sizes, respectively with irritability. AN was associated negatively with headstrong. The findings indicated evidence of unique positive associations of low effect size between irritability and BN, and a unique positive association of small effect size between AN and irritability. Seen together with their standardized beta coefficients for the ODD dimensions when they were examined separately, the negative findings for the associations involving headstrong and AN are better interpreted as headstrong having a suppression effect on the relation between irritability and AN (thereby increasing the strength of this association) than a unique negative association between headstrong and AN.
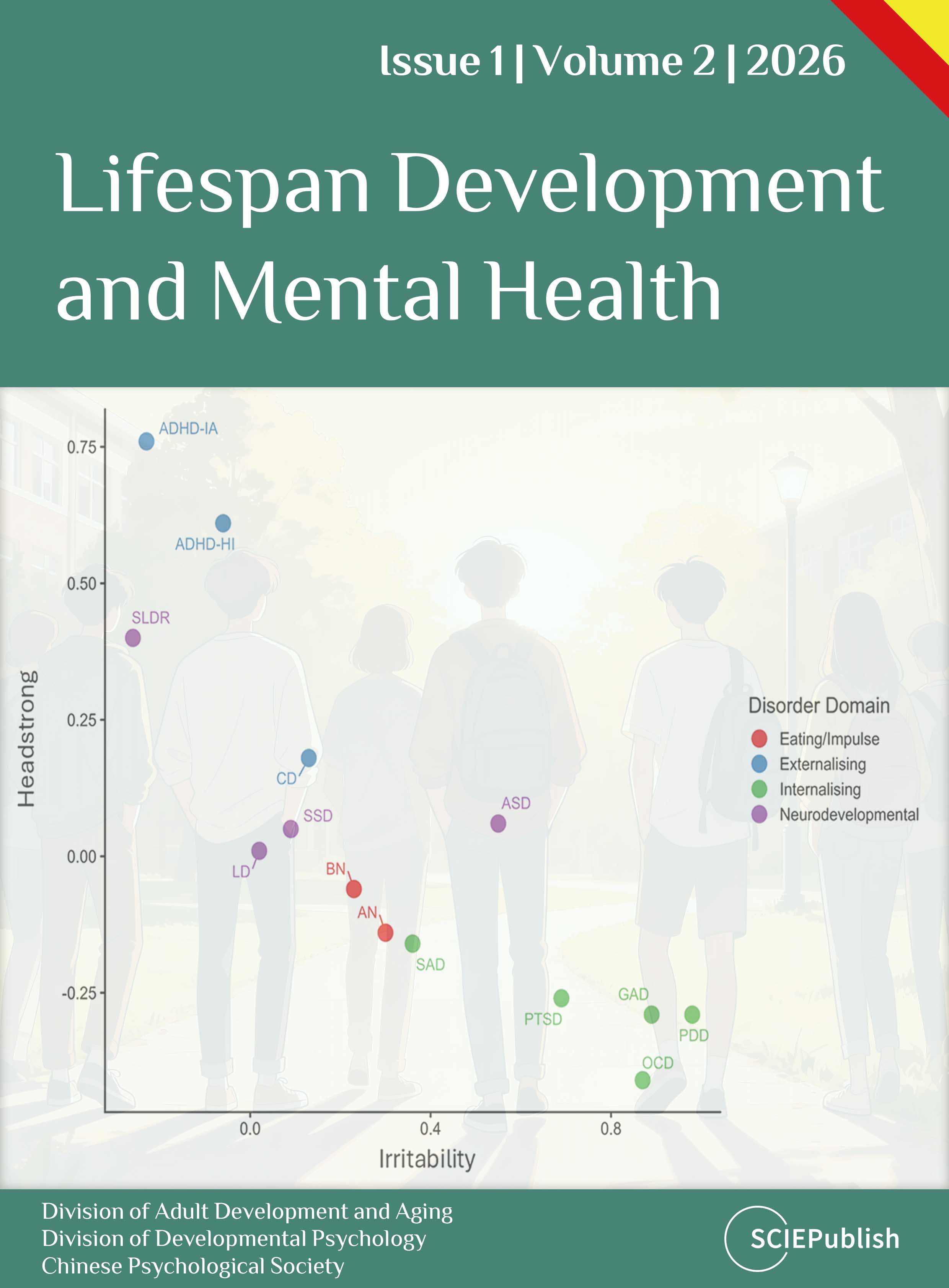
To visualise the relative positioning of adolescent psychological disorders across oppositional defiant disorder (ODD) dimensions, a two-dimensional coordinate plot was generated using standardized path coefficients derived from structural equation modelling (SEM). Separate SEMs were estimated in which a combined Irritability/Headstrong coefficient was entered as a predictors of each disorder (see supplementary Table S2 and Figure S2). Standardized I/H together coefficients (see Table 2) were used to define the x-axis and y-axis. This approach allows disorders to be positioned within a common dimensional space that reflects their overall association with each ODD dimension. As such, proximity between disorders in the plot reflects similarity in their dimensional profiles rather than unique effects conditional on the other ODD dimension.
5. Discussion
The findings of this study showed that in the SRA with either irritability or headstrong in the model, all disorders were associated positively with irritability and headstrong. Associations with the internalizing disorders, externalizing disorders, ASD, and BN were either high or medium effect sizes, with both irritability or headstrong, and the associations for SLDR, LD, SSD, and AN were of small effect sizes, with both irritability or headstrong. AN was also associated with a medium effect size with irritability.
With both the ODD dimensions in the model, the MRA showed that all the internalizing disorders were associated positively and uniquely with either large of medium effect sizes with irritability, and showed no associations with headstrong. All the externalizing disorders were associated uniquely with large effect sizes with headstrong, and while CD also showed a positive, but small association with irritability, the other disorders (ADHDHI and ADHDIA) showed no associations with irritability. Also, although ASD was associated uniquely with a large effect size with irritability, it also showed low unique effect size association with headstrong. The other neurodevelopmental disorders (SLDR, LD, and SSD) showed little or no associations with both irritability and headstrong. As for the eating disorders, BN and AN irritability showed a unique positive association of low and medium effect size with irritability, and BN showed a unique positive association of low effect size with headstrong.
The LRA with both the ODD dimensions in the model showed that for the internalizing disorders, there was evidence of positive associations of large or medium effect sizes for all the internalizing disorders with irritability, and negative associations of low effect sizes with headstrong. As the standardized beta for headstrong for the predictions of the internalizing disorders were significant and positive when examined separately, these negative associations are better interpreted as reflecting suppression effects that increased the strengths of the associations between internalizing disorders and irritability. Overall, therefore, the internalizing disorders were uniquely and positively associated with large or medium effect sizes, with only irritability.
The LRA with both the ODD dimensions showed that for the externalizing disorders, there was evidence of a positive association of a small effect size for CD, and a positive association of a large effect size for ADHDIA and ADHDHI with headstrong. CD was also positive associated with small effect size with irritability. ADHDIA was associated negatively with small effect size with irritability, and ADHDHI was not associated with irritability. As the standardized beta for irritability for the predictions of the externalizing disorders was significant and positive when examined separately, the negative association involving irritability and ADHDIA is better interpreted as reflecting a suppression effect that increased the strength of the association between ADHDIA and headstrong. Overall, therefore, ADHDIA and ADHDHI were uniquely and positively associated with large effect sizes, with only headstrong. CD was uniquely and positively associated with a low effect size with both headstrong and irritability.
In relation to the neurodevelopmental disorders, the LRA with both ODD dimensions in the analysis showed that, for ASD, there was evidence of a positive association of large effect size with irritability and no significant association with headstrong. LD and SSD showed no significant associations with both irritability and headstrong. SLDR was associated significantly and positively with a medium effect size with headstrong, and significantly and negatively with a small effect size with irritability. As the standardized beta for irritability for the predictions of SLDR was significant and positive when examined separately, the negative association involving irritability and SLDR is better interpreted as reflecting a suppression effect that increased the strength of the association between SLDR and headstrong. Overall, therefore, ASD was uniquely and positively associated with a large effect size, with only irritability. SLDR was uniquely and positively associated with a medium effect size with headstrong. LD and SSD were not uniquely associated with both irritability and headstrong. In this respect, an alternative explanation for the lack of significant associations is that these problems often manifest in subtle and context-dependent ways and are therefore less noticeable to parents than behavioral or emotional problems. Parents are generally better at reporting externalizing behavior or clear mood problems than specific language or articulation difficulties, which often occur mainly in school or formal communication settings. When measurement is based only on parent reports, this may lead to an underestimation of the severity and variability of language and speech disorders. As a result, score variability is limited, making statistical associations with ODD dimensions difficult to detect, even if such associations actually exist.
In relation to the eating disorders, the LRA with both the ODD dimensions in the analysis, showed that for BN was associated positively with low effect size with irritability; and AN was associated positively with medium effect size with irritability. BN was associated significantly with headstrong; and AN was associated negatively with low effect size with headstrong. As the standardized beta for irritability for the predictions of AN was significant and positive when examined separately, the negative association involving headstrong and AN is better interpreted as reflecting a suppression effect that increased the strength of the association between AN and irritability.
Overall, therefore, both the MRA and LRA indicated similar unique relationships, except for ASD and LD. While the MRA indicated a unique positive association for ASD and LD with headstrong, the LRA showed no significant associations. Notwithstanding the high degrees of comparability across the MRA and LRA, unlike the results for the MRA, the results for the LRA indicated a potential suppression effect. More specifically, in virtually all instances, the associations for irritability with the disorders (when present) were suppressed by headstrong that resulted in stronger associations between irritability and the disorders; the associations for headstrong with the disorders (when present) were suppressed by irritability that resulted in stronger associations between headstrong and the disorders. Our findings also mean that the LRA was able to consider suppression effects, whereas the MRA was unable to do so.
The findings in this study in the MRA replicate findings in this area. Like the findings in this study, previous findings that have examined observed scores have also indicted that irritability is generally more strongly associated with internalizing disorders, and that headstrong is generally more strongly associated with externalizing disorders [2,5,7]. However, our findings are inconsistent with Klos et al.’s [11] findings that both the ODD irritability and headstrong dimensions are associated more with the externalizing problems than internalizing problems. Our findings also differ from the findings reported by Mikolajewski et al. [12] that both the ODD dimensions predicted uniquely antisocial behavior (alcohol use disorder, cannabis use disorder; and adult antisocial behavior) and overall externalizing problems, and that the irritable dimension has no unique associations with specific internalizing disorders (major depressive disorder, social phobia, specific phobia, and panic disorder). Considering that the current study used latent scores (that are free of error variance), accounted for suppression effects, and examined disorders that reflected the DSM-5 disorders with the same name, it can be argued that the findings in the current study provide a more credible and better understanding of the relationships of the ODD irritability and headstrong dimensions with other disorders. This also means that for a better understanding of these relationships, studies need to examine latent scores, account for suppression effects, and examine disorders that reflect the DSM-5 disorders with the same name. Currently, there is relatively little data in this respect.
The current study extended existing findings in this area. First, it showed that despite being an externalizing disorder, CD was uniquely associated with both ODD headstrong and ODD irritability. Second, all the findings for the neurodevelopmental disorders and the eating disorders are new, as these have not been examined in previous studies. They showed that with the exception of ASD, the other neurodevelopmental disorders (SLDR, LD, and SSD) were not associated with either irritability or headstrong. ASD, AN and BN were associated with irritability. Third, as already mentioned, our findings showed that associations for irritability with the disorders (when present) were suppressed by headstrong that resulted in stronger associations between irritability and the disorders; and the associations for headstrong with the disorders (when present) were suppressed by irritability that resulted in stronger associations between headstrong and the disorders. Notwithstanding these novel findings, although we have tended to interpret negative associations as suppression effects, it is conceivable that they could reflect measurement problems or model misspecification.
Overall, the findings in this study provide more clearer understanding of the associations for the ODD dimensions with the other disorders, and therefore offer more meaningful implications for theory, clinical classification, and practice. Considering that we have advocated support for studies using latent scores, we will discuss the theoretical, taxonomic, and clinical implications based on the results from the LRA analyses.
6. Theoretical Implications
As our findings showed that the internalizing disorders (GAD, SAD, PDD, OCD and PTSD), BN and ASD were uniquely associated with ODD irritability, and were not associated with ODD headstrong, it can be argued that irritability may explain the comorbidity of ODD with the internalizing disorders, ASD and BN, and potentially, the comorbidity between these internalizing disorders with each other and with ASD and BN, and between ASD and BN. Also, as all the externalizing disorders (CD, ADHDIA, and ADHDHI) were uniquely associated with ODD headstrong, and not with ODD irritability, it can be argued that ODD headstrong is more important than ODD irritability for explaining the comorbidity of ODD with these externalizing disorders, and potentially, the comorbidity between these externalizing disorders. The absence of unique associations for SLDR, LD, and SSD with either irritability or headstrong, suggest that ODD is unlikely to be related to these disorders.
Our findings and interpretations raise the possibility that both irritability and headstrong may be transdiagnostic (a factor that may account for the comorbidity of symptoms between several disorders), playing a dominant influence on the comorbidity of internalizing (and possibly eating disorders) and externalizing disorders, respectively. At present, including research not focused on ODD, the transdiagnostic characteristic of irritability in relation of internalizing disorders has been supported [54,55]. Indeed, irritability is featured in the Research Domains Criteria (RDoC [56]) and the Hierarchical Taxonomy of Psychopathology (HiTOP [57]) transdiagnostic classification systems. The RDoC views irritability as a biobehavioral construct of frustrative nonreward in the negative valence-systems domain; and in the HiTOP, it is included as a distress subfactor of the internalizing spectrum [58].
To date, irritability has been distinguished into tonic irritability (persistent anger, easily triggered annoyance) and phasic irritability (temper outbursts [59]), and there are data showing that tonic irritability is associated with internalizing disorders, and phasic irritability is associated with externalizing disorders [59,60,61]. Given that, we used the ODD symptoms for “temper”, “touchy” and “angry”, it can be assumed that the irritability construct used in the current study reflected overall irritability (tonic plus phasic). Thus, it can be assumed that the findings reported here for irritability are relevant to general irritability (i.e., both tonic and phasic irritability). Relatedly, it may be worth noting that, as general irritability or both phasic and tonic symptoms of irritability are the core dimensions of the newly proposed disruptive mood dysregulation disorder (DMDD [13]), our findings and interpretation for the irritability are likely to be relevant for DMDD. Clearly, more studies are needed in this respect.
In contrast to irritability, there has been little discussion on headstrong as a transdiagnostic factor. It has been suggested that impulsivity, disinhibition, rumination, emotion dysregulation, social rejection, social-information-processing deficits, and biological vulnerabilities (such as dopaminergic and serotonergic vulnerabilities) are major transdiagnostic factors for externalizing disorders [62,63,64,65]. A systematic review revealed that for externalizing psychopathologies, executive functioning deficits, earlier pubertal timing, being male (biological factors), stressful life events (socio-environmental factor), and high neuroticism and low effortful control (psychological factors) are major transdiagnostic risk factors.
Effortful control refers to self-regulation of emotional reactivity and behavior. High self-control reflects high ability to adjust and control one’s behavior to situational demands in a flexible and willful manner. Individuals with low effortful control would have difficulties inhibiting impulsive behaviors, and managing strong emotions like anger, and following directions, which are reflective of being headstrong (being stubborn, willful, and resistant to control). Existing findings indicate that low effortful control is robustly associated with externalizing behaviors and disorders across the lifespan [66,67,68]. Given such findings it can be expected that because of its association with low effortful control is likely to be a transdiagnostic risk factor for externalizing disorders through poor behavioral and emotional regulation [69].
7. Clinical Implications
Although DSM-5 ODD has three dimensions (anger/irritable mood, argumentative/defiant, and vindictiveness, the different symptom groups are not considered for the purpose of diagnosis of ODD, i.e., there are no different ODD types based on the ODD symptom groups. Instead, the ODD diagnosis is quantified as mild, moderate, or severe, based on the number of settings in which symptoms occur. However, given our findings that ODD irritability is generally associated with internalizing disorders and eating disorders, and ODD headstrong is generally associated with externalizing disorders and neurodevelopmental disorders, we believe that it would be useful to consider the ODD symptom groups for diagnostic purposes. A similar approach to that for the diagnosis of ADHD presentations would be useful, i.e., identifying ODD-irritability and ODD-headstrong types. This could facilitate the diagnostic process, particularly by identifying potential comorbidities. Thus, we recommend that future editions of the DSM consider this possibility, as it could have implications for diagnosis and, consequently, treatment. Additionally, as we showed associations of ODD in a group of adolescents, it can be argued that, as embraced in DSM-5, ODD is a relevant diagnosis in this age group.
8. Study Limitations and Directions for Further Studies
This study has a number of limitations that need to be kept in mind when considering the findings and interpretations. As we used cross-sectional data, all our findings cannot be interpreted in causal terms. Although the participants in this study were from a psychology clinic, their clinical status was unknown. Additionally, the sample was not based on a random selection. Thus, there are limitations regarding the generalization of the findings to adolescents with a clinical diagnosis (including those with ODD) and older and younger age groups. Similarly, as data were obtained using the CAPP-PRF, they cannot be generalized to other measures or data obtained using clinical interviews. Additionally, it is possible that the findings may have been confounded by possible content overlap between ODD items and items from other disorders, which could in part explain the observed associations. Considering these limitations, there is a need for more studies, using longitudinal data and multiple methods, and involving different ages and clinically diagnosed groups. Notwithstanding these limitations, we have offered a number of novel findings, in particular the need to examine latent scores, and have accounted for suppression effects when examining unique relationships between the ODD dimensions and other DSM-5 disorders. This has not been given much attention in past research in this area.
Supplementary Materials
The following supporting information can be found at: https://www.sciepublish.com/article/pii/884, Figure S1: Schematic diagram illustrating the SEM model used to examine the unique associations of ADHDIA with the ODD dimensions; Figure S2: Dimensional Positioning of the Adolescent Disorders Based non the SEM Results; Table S1: Mean and Standard Deviations for the ODD Symptoms Used in the Study; Table S2: Frequencies of Comorbidity Based on Diagnostic Symptom Threshold Number.
Statement of the Use of Generative AI and AI-Assisted Technologies in the Writing Process
During the preparation of this manuscript, the author(s) used ChatGPT model 5.1 in order to edit the manuscript. After using this tool/service, the author(s) reviewed and edited the content as needed and take(s) full responsibility for the content of the published article.
Author Contributions
Conceptualization, Methodology, Software, Validation, Formal Analysis, Investigation, Resources, Data Curation, Writing—Original Draft Preparation, Supervision and Project Administration, R.G. Writing—Review & Editing, D.Z., S.L. and S.H.; Visualization, D.Z.
Ethics Statement
The study was conducted according to the guidelines of the Declaration of Helsinki, and approved by the Institutional Review Board (or Ethics Committee) of The University of Western Australia (UWA Human Research Ethics Approval Number—ROAP 2023/ET000965, 27 March 2025). All participants provided informed consent.
Informed Consent Statement
Informed consent was obtained from all subjects involved in the study.
Data Availability Statement
Data can be made available upon reasonable request.
Funding
The author(s) declare that no financial support was received for the research, authorship, and/or publication of this article.
Declaration of Competing Interest
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
References
- Aebi M, Müller UC, Asherson P, Banaschewski T, Buitelaar J, Ebstein R, et al. Predictability of oppositional defiant disorder and symptom dimensions in children and adolescents with ADHD combined type. Psychol. Med. 2010, 40, 2089–2100. DOI:10.1017/S0033291710000590 [Google Scholar]
- Burke J, Loeber R. Oppositional defiant disorder and the explanation of the comorbidity between behavioral disorders and depression. Clin. Psychol. Sci. Pract. 2010, 17, 319–326. DOI:10.1111/j.1468-2850.2010.01223.x [Google Scholar]
- Gomez R, Stavropoulos V, Van Doorn G. Factor structure of teacher ratings of the ODD symptoms in children. Psychiatic Q. 2018, 89, 219–234. DOI:10.1007/s11126-017-9527-6 [Google Scholar]
- Jungersen CM, Lonigan CJ. Dimensionality of oppositional defiant disorder symptoms across elementary-school grades. Child Psychiatry Hum. Dev. 2024, 55, 1103–1114. DOI:10.1007/s10578-022-01474-w [Google Scholar]
- Rowe R, Costello EJ, Angold A, Copeland WE, Maughan B. Developmental pathways in oppositional defiant disorder and conduct disorder. J. Abnorm. Psychol. 2010, 119, 726–738. DOI:10.1037/a0020798 [Google Scholar]
- Burke JD. An affective dimension within ODD symptoms among boys: Personality and psychopathology outcomes into early adulthood. J. Child Psychol. Psychiatry Allied Discip. 2012, 53, 1176–1183. DOI:10.1111/j.1469-7610.2012.02598.x [Google Scholar]
- Stringaris A, Goodman R. Longitudinal outcome of youth oppositionality: Irritable, headstrong, and hurtful behaviors have distinctive predictions. J. Am. Acad. Child Adolesc. Psychiatry 2009, 48, 404–412. DOI:10.1097/CHI.0b013e3181984f30 [Google Scholar]
- Leadbeater BJ, Homel J. Irritable and defiant sub-dimensions of ODD: Their stability and prediction of internalizing symptoms and conduct problems from adolescence to young adulthood. J. Abnorm. Child Psychol. 2015, 43, 407–421. DOI:10.1007/s10802-014-9908-3 [Google Scholar]
- Boylan K, Vaillancourt T, Boyle M, Szatmari P. Comorbidity of internalizing disorders in children with oppositional defiant disorder. Eur. Child Adolesc. Psychiatry 2007, 16, 484–494. DOI:10.1007/s00787-007-0624-1 [Google Scholar]
- Nobakht HN, Steinsbekk S, Wichstrøm L. Development of symptoms of oppositional defiant disorder from preschool to adolescence: The role of bullying victimization and emotion regulation. J. Child Psychol. Psychiatry 2024, 65, 343–353. DOI:10.1111/jcpp.13845 [Google Scholar]
- Klos S, Thöne AK, Döpfner M, Görtz-Dorten A. Self-Rated Symptoms of Oppositional Defiant Disorder and Conduct Disorder: Factor Structure, Reliability, and Validity in a Clinical Sample of Adolescents. Child Psychiatry Hum. Dev. 2024, 56, 1147–1160. DOI:10.1007/s10578-024-01802-2 [Google Scholar]
- Mikolajewski AJ, Taylor J, Iacono WG. Oppositional defiant disorder dimensions: Genetic influences and risk for later psychopathology. J. Child Psychol. Psychiatry 2017, 58, 702–710. DOI:10.1111/jcpp.12683 [Google Scholar]
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, 5th ed.; Text Revision (DSM-5-TR); American Psychiatric Association: Washington, DC, USA, 2022. DOI:10.1176/appi.books.9780890425787 [Google Scholar]
- Achenbach TM, Rescorla LA. Manual for the ASEBA School-Age Forms & Profiles; University of Vermont, Research Center for Children, Youth, and Families: Burlington, VT, USA, 2001. [Google Scholar]
- Stoddard J, Stringaris A, Brotman MA, Montville D, Pine DS, Leibenluft E. Irritability in child and adolescent anxiety disorders. Depress. Anxiety 2014, 31, 566–573. DOI:10.1002/da.22151 [Google Scholar]
- Vidal-Ribas P, Stringaris A. How and why Are irritability and depression linked? Child Adolesc. Psychiatr. Clin. North Am. 2021, 30, 401–414. DOI:10.1016/j.chc.2020.10.009 [Google Scholar]
- Biederman J, Faraone SV, Milberger S, Jetton JE, Chen L, Mick E, et al. Is childhood oppositional defiant disorder a precursor to adolescent conduct disorder? Findings from a four-year follow-up study of children with ADHD. J. Am. Acad. Child Adolesc. Psychiatry 1996, 35, 1193–1204. DOI:10.1097/00004583-199609000-00017 [Google Scholar]
- Francés L, Quintero J, Fernández A, Ruiz A, Caules J, Fillon G, et al. Current state of knowledge on the prevalence of neurodevelopmental disorders in childhood according to the DSM-5: A systematic review in accordance with the PRISMA criteria. Child Adolesc. Psychiatry Ment. Health 2022, 16, 27. DOI:10.1186/s13034-022-00462-1 [Google Scholar]
- Yang Y, Zhao S, Zhang M, Xiang M, Zhao J, Chen S, et al. Prevalence of neurodevelopmental disorders among US children and adolescents in 2019 and 2020. Front. Psychol. 2022, 13, 997648. DOI:10.3389/fpsyg.2022.997648 [Google Scholar]
- Fisher M, Golden NH, Katzman DK, Kreipe RE, Rees J, Schebendach J, et al. Eating disorders in adolescents: A background paper. J. Adolesc. Health 1995, 16, 420–437. DOI:10.1016/1054-139X(95)00069-5 [Google Scholar]
- Johnston O, Fornai G, Cabrini S, Kendrick T. Feasibility and acceptability of screening for eating disorders in primary care. Fam. Pract. 2007, 24, 511–517. DOI:10.1093/fampra/cmm029 [Google Scholar]
- Silén M, Skytt B, Engström M. Relationships between structural and psychological empowerment, mediated by person-centred processes and thriving for nursing home staff. Geriatr. Nurs. 2019, 40, 67–71. DOI:10.1016/j.gerinurse.2018.06.016 [Google Scholar]
- Augustine L, Lygnegård F, Granlund M. Trajectories of participation, mental health, and mental health problems in adolescents with self-reported neurodevelopmental disorders. Disabil. Rehabil. 2022, 44, 1595–1608. DOI:10.1080/09638288.2021.1955304 [Google Scholar]
- Eyre O, Hughes RA, Thapar AK, Leibenluft E, Stringaris A, Davey Smith G, et al. Childhood neurodevelopmental difficulties and risk of adolescent depression: The role of irritability. J. Child Psychol. Psychiatry 2019, 60, 866–874. DOI:10.1111/jcpp.13053 [Google Scholar]
- Hansen BH, Oerbeck B, Skirbekk B, Petrovski BÉ, Kristensen H. Neurodevelopmental disorders: Prevalence and comorbidity in children referred to mental health services. Nord. J. Psychiatry 2018, 72, 285–291. DOI:10.1080/08039488.2018.1444087 [Google Scholar]
- Jenkins PE, Hoste RR, Doyle AC, Eddy K, Crosby RD, Hill L, et al. Health-related quality of life among adolescents with eating disorders. J. Psychosom. Res. 2014, 76, 1–5. DOI:10.1016/j.jpsychores.2013.11.006 [Google Scholar]
- Johnson JG, Cohen P, Kasen S, Brook JS. Eating disorders during adolescence and the risk for physical and mental disorders during early adulthood. Arch. Gen. Psychiatry 2002, 59, 545–552. DOI:10.1001/archpsyc.59.6.545 [Google Scholar]
- Nadder TS, Rutter M, Silberg JL, Maes HH, Eaves LJ. Genetic effects on the variation and covariation of attention deficit-hyperactivity disorder (ADHD) and oppositional-defiant disorder/conduct disorder (ODD/CD) symptomatologies across informant and occasion of measurement. Psychol. Med. 2002, 32, 39–53. DOI:10.1017/S0033291701004792 [Google Scholar]
- Tuvblad C, Zheng M, Raine A, Baker LA. A common genetic factor explains the covariation among ADHD ODD and CD symptoms in 9–10 year old boys and girls. J. Abnorm. Child Psychol. 2009, 37, 153–167. DOI:10.1007/s10802-008-9278-9 [Google Scholar]
- Gomez R, Stavropoulos V, Watson S, Brown T, Chen W. Inter-relationships between ADHD, ODD and impulsivity dimensions in emerging adults revealed by network analysis: Extending the ‘trait impulsivity hypothesis’. Heliyon 2022, 8, e10712. DOI:10.1016/j.heliyon.2022.e10712. [Google Scholar]
- Mandy W, Roughan L, Skuse D. Three dimensions of oppositionality in autism spectrum disorder. J. Abnorm. Child Psychol. 2014, 42, 291–300. DOI:10.1007/s10802-013-9778-0 [Google Scholar]
- Drabick DAG, Gadow KD, Loney J. Source-specific oppositional defiant disorder: Comorbidity and risk factors in referred elementary schoolboys. J. Am. Acad. Child Adolesc. Psychiatry 2007, 46, 92–101. DOI:10.1097/01.chi.0000242245.00174.90 [Google Scholar]
- Munkvold L, Lundervold A, Lie SA, Manger T. Should there be separate parent and teacher-based categories of ODD? Evidence from a general population. J. Child Psychol. Psychiatry 2009, 50, 1264–1272. DOI:10.1111/j.1469-7610.2009.02091.x [Google Scholar]
- Mason TB, Smith KE. Psychiatric comorbidity associated with eating disorders in 9-to 10-year-old children. Can. J. Psychiatry 2022, 67, 316–319. DOI:10.1177/07067437211026485 [Google Scholar]
- Pauli‐Pott U, Becker K, Albayrak Ö, Hebebrand J, Pott W. Links between psychopathological symptoms and disordered eating behaviors in overweight/obese youths. Int. J. Eat. Disord. 2013, 46, 156–163. DOI:10.1002/eat.22055 [Google Scholar]
- Favaro A, Zanetti T, Tenconi E, Degortes D, Ronzan A, Veronese A, et al. The relationship between temperament and impulsive behaviors in eating disordered subjects. Eat. Disord. 2005, 13, 61–70. DOI:10.1080/10640260590893647 [Google Scholar]
- Dingemans A, Danner U, Parks M. Emotion regulation in binge eating disorder: A review. Nutrients 2017, 9, 1274. DOI:10.3390/nu9111274 [Google Scholar]
- Eichen DM, Chen E, Boutelle KN, McCloskey MS. Behavioral evidence of emotion dysregulation in binge eaters. Appetite 2017, 111, 1–6. DOI:10.1016/j.appet.2016.12.021 [Google Scholar]
- Howells RL, Dunn LC, Carter JC. The relationship between difficulties in the regulation of positive and negative emotions and binge-eating symptoms in young adults. Eat. Behav. 2024, 52, 101839. DOI:10.1016/j.eatbeh.2023.101839 [Google Scholar]
- Cohen J, Cohen P, West SG, Aiken LS. Applied Multiple Regression/Correlation Analysis for the Behavioral Sciences, 3rd ed.; Lawrence Erlbaum Associates Publishers: Hillsdale, NJ, USA, 2003. [Google Scholar]
- Tzelgov J, Henik A. Suppression situations in psychological research: Definitions, implications, and applications. Psychol. Bull. 1991, 109, 524–536. DOI:10.1037/0033-2909.109.3.524 [Google Scholar]
- Cheung MWL. A model for integrating fixed-, random-, and mixed-effects meta-analyses into structural equation modeling. Psychol. Methods 2008, 13, 182–202. DOI:10.1037/a0013163 [Google Scholar]
- Njardvik U, Wergeland GJ, Riise EN, Hannesdottir DK, Öst LG. Psychiatric comorbidity in children and adolescents with ADHD: A systematic review and meta-analysis. Clin. Psychol. Rev. 2025, 118, 102571. DOI:10.1016/j.cpr.2025.102571 [Google Scholar]
- Langsford S, Houghton S, Douglas G. PsychProfiler v5 Manual; Psychological and Educational Consultancy Services: Subiaco, Australia, 2014. [Google Scholar]
- Enders CK, Bandalos DL. The relative performance of full information maximum likelihood estimation for missing data in structural equation models. Struct. Equ. Model. 2001, 8, 430–457. DOI:10.1207/S15328007SEM0803_5 [Google Scholar]
- Campbell OL, Bann D, Patalay P. The gender gap in adolescent mental health: A cross-national investigation of 566,829 adolescents across 73 countries. SSM-Popul. Health 2021, 13, 100742. DOI:10.1016/j.ssmph.2021.100742. [Google Scholar]
- Van Droogenbroeck F, Spruyt B, Keppens G. Gender differences in mental health problems among adolescents and the role of social support: Results from the Belgian health interview surveys 2008 and 2013. BMC Psychiatry 2018, 18, 6. DOI:10.1186/s12888-018-1591-4 [Google Scholar]
- Yoon Y, Eisenstadt M, Lereya ST, Deighton J. Gender difference in the change of adolescents’ mental health and subjective wellbeing trajectories. Eur. Child Adolesc. Psychiatry 2023, 32, 1569–1578. DOI:10.1007/s00787-022-01961-4 [Google Scholar]
- Muthen LK, Muthen BO. Mplus User’s Guide, 7th ed.; Muthén & Muthén: Los Angeles, CA, USA, 2012. [Google Scholar]
- Cohen JE. Statistical Power Analysis for the Behavioral Sciences; Lawrence Erlbaum Associates, Inc.: Hillsdale, NJ, USA, 1988. [Google Scholar]
- Cohen J, Cohen P. Applied Multiple Regression/Correlation Analysis for the Behavioral Sciences; Erlbaum: Hillsdale, NJ, USA, 1983. [Google Scholar]
- Gaylord-Harden NK, Cunningham JA, Holmbeck GN, Grant KE. Suppressor effects in coping research with African American adolescents from low-income communities. J. Consult. Andcllinical Psychol. 2010, 78, 843–855. DOI:10.1037/a0020063 [Google Scholar]
- Hu LT, Bentler PM. Fit Indices in covariance structure modeling: Sensitivity to underparameterized model misspecification. Psychol. Methods 1998, 3, 424–453. DOI:10.1037/1082-989X.3.4.424 [Google Scholar]
- Evans SC, Burke JD, Roberts MC, Fite PJ, Lochman JE, de la Peña FR, et al. Irritability in child and adolescent psychopathology: An integrative review for ICD-11. Clin. Psychol. Rev. 2017, 53, 29–45. DOI:10.1016/j.cpr.2017.01.004 [Google Scholar]
- Leibenluft E, Allen LE, Althoff RR, Brotman MA, Burke JD, Carlson GA, et al. Irritability in youths: A critical integrative review. Am. J. Psychiatry 2024, 181, 275–290. DOI:10.1176/appi.ajp.20230256 [Google Scholar]
- Cuthbert BN. The role of RDoC in future classification of mental disorders. Dialogues Clin. Neurosci. 2020, 22, 81–85. DOI:10.31887/DCNS.2020.22.1/bcuthbert [Google Scholar]
- Kotov R, Krueger RF, Watson D, Achenbach TM, Althoff RR, Bagby RM, et al. The Hierarchical Taxonomy of Psychopathology (HiTOP): A dimensional alternative to traditional nosologies. J. Abnorm. Psychol. 2017, 126, 454–477. DOI:10.1037/abn0000258 [Google Scholar]
- Klein DN, Dougherty LR, Kessel EM, Silver J, Carlson GA. A transdiagnostic perspective on youth irritability. Curr. Dir. Psychol. Sci. 2021, 30, 437–443. DOI:10.1177/09637214211035101 [Google Scholar]
- Leibenluft E. Pediatric irritability: A systems neuroscience approach. Trends Cogn. Sci. 2017, 21, 277–289. DOI:10.1016/j.tics.2017.02.002 [Google Scholar]
- Hawes MT, Carlson GA, Finsaas MC, Olino TM, Seely JR, Klein DN. Dimensions of irritability in adolescents: Longitudinal associations with psychopathology in adulthood. Psychol. Med. 2020, 50, 2759–2767. DOI:10.1017/S0033291719002903 [Google Scholar]
- Silver J, Carlson GA, Olino TM, Perlman G, Mackin D, Kotov R, et al. Differential outcomes of tonic and phasic irritability in adolescent girls. J. Child Psychol. Psychiatry 2021, 62, 1220–1227. DOI:10.1111/jcpp.13402 [Google Scholar]
- Beauchaine TP, Hinshaw SP, Pang KL. Comorbidity of attention-deficit/hyperactivity disorder and early-onset conduct disorder: Biological, environmental, and developmental mechanisms. Clin. Psychol. Sci. Pract. 2010, 17, 327–336. DOI:10.1111/j.1468-2850.2010.01224.x [Google Scholar]
- Burke JD, Loeber R, Birmaher B. Oppositional defiant disorder and conduct disorder: A review of the past 10 years, part II. J. Am. Acad. Child Adolesc. Psychiatry 2002, 41, 1275–1293. DOI:10.1097/00004583-200211000-00009 [Google Scholar]
- Dodge KA. Social-cognitive mechanisms in the development of conduct disorder and depression. Annu. Rev. Psychol. 1993, 44, 559–584. DOI:10.1146/annurev.ps.44.020193.003015 [Google Scholar]
- Krueger RF, Markon KE. Reinterpreting comorbidity: A model-based approach to understanding and classifying psychopathology. Annu. Rev. Clin. Psychol. 2006, 2, 111–133. DOI:10.1146/annurev.clinpsy.2.022305.095213 [Google Scholar]
- Meehan KB, De Panfilis C, Cain NM, Clarkin JF. Effortful control and externalizing problems in young adults. Personal. Individ. Differ. 2013, 55, 553–558. DOI:10.1016/j.paid.2013.04.019 [Google Scholar]
- Mischel W, Ayduk O, Berman MG, Casey BJ, Gotlib IH, Jonides J, et al. ‘Willpower’ over the life span: Decomposing self-regulation. Soc. Cogn. Affect. Neurosci. 2011, 6, 252–256. DOI:10.1093/scan/nsq081 [Google Scholar]
- Muris P, Meesters C, Blijlevens P. Self-reported reactive and regulative temperament in early adolescence: Relations to internalizing and externalizing problem behavior and “Big Three” personality factors. J. Adolesc. 2007, 30, 1035–1049. DOI:10.1016/j.adolescence.2007.03.003 [Google Scholar]
- Thompson SF, Zalewski M, Kiff CJ, Moran L, Cortes R, Lengua LJ. An empirical test of the model of socialization of emotion: Maternal and child contributors to preschoolers’ emotion knowledge and adjustment. Dev. Psychol. 2020, 56, 418–430. DOI:10.1037/dev0000860 [Google Scholar]