Found 26 results
Open Access
Article
20 August 2025Mitochondrial Lon Peptidase 1 Controls Diaphragm and Lung Development in a Context-Dependent Manner
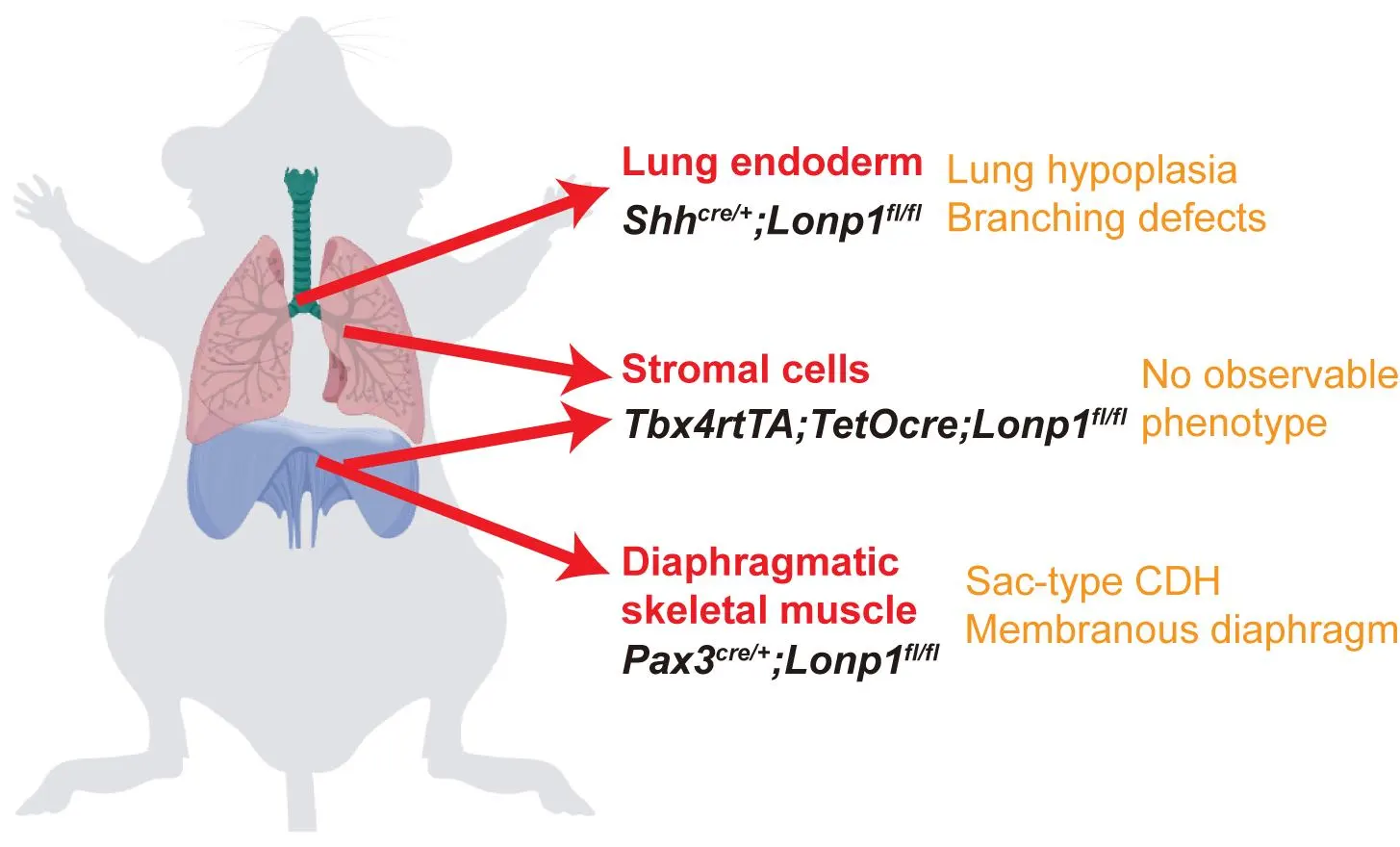
Congenital Diaphragmatic Hernia (CDH) is a rare neonatal disorder causing diaphragmatic defects and cardiopulmonary hypoplasia, traditionally attributed to mechanical compression from organ herniation. However, emerging evidence suggests genetic mutations may independently impair lung development, prompting debate over CDH etiology. Here, we investigated the requirement of mitochondrial function guarded by LON peptidase 1 (Lonp1), a CDH risk gene, in either diaphragm or lung development. Lonp1 loss in skeletal muscles of the diaphragm led to its thinning and membranization, recapitulating the pathology of sac-type CDH. On the other hand, lung-specific inactivation caused severe hypoplasia with defective branching morphogenesis, independent of diaphragm anomalies. Molecularly, Lonp1 disruption dysregulated key transcription factors and signaling pathways known to be critical for early lung development. Our findings here revealed that mitochondrial defects contribute to the pathogenesis of CDH in an organ and cell type specific manner, opening new avenues for drug and therapeutic development.
Open Access
Article
25 June 2025Time Is Lung: Inpatient Transbronchial Lung Cryobiopsy Decreases Wait Time to Treatment Initiation for Newly Diagnosed Interstitial Lung Disease
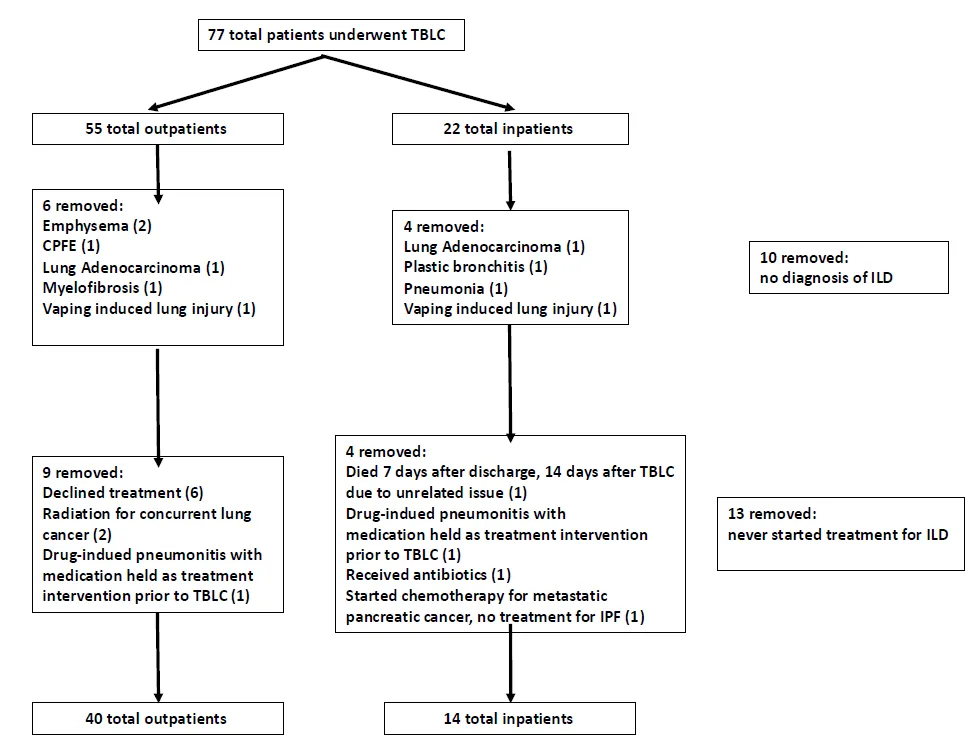
Although performing lung biopsies on hospitalized patients with interstitial lung disease (ILD) has risk, initial studies have shown transbronchial lung cryobiopsy (TBLC) may be safely performed in this patient group. Data evaluating the value of this intervention in establishing a diagnosis and impacting management is lacking. We present a comparison of TBLC for inpatients and outpatients and provide data on the impact on medical therapy initiation and wait times from consultation to biopsy and treatment. Demographic data, pulmonary function values, chest imaging patterns, procedural information, diagnosis, and medical therapy changes, defined as medication initiation, adjustment, or cessation guided by TBLC results, were recorded from enrolled patients with newly identified ILD. Changes in medical therapy were the primary outcome. Time from consultation to biopsy and treatment was the secondary outcome. Fifty-four (54) patients (40 outpatient, 14 inpatient) were included. Inpatients underwent biopsy 2.5 ± 4.4 days after consultation compared to 15.5 ± 16.1 days for outpatients (p < 0.001). Medical therapy changes occurred 10.3 ± 7.9 days after biopsy for inpatients compared to 34.6 ± 37.0 days for outpatients (p < 0.001). There were no significant differences in medical therapy changes between the groups (p = 0.45). Our initial study suggests that performing TBLC on inpatients with newly identified ILD decreases wait times to treatment initiation and diagnosis. Efforts to understand the impact of a decreased wait time on ILD prognosis, including the development of progressive disease or fibrosis, symptom evolution, and quality of life, require further evaluation.
Open Access
Article
15 May 2025Enhanced Spatial Transcriptomics Analysis of Mouse Lung Tissues Reveals Cell-Specific Gene Expression Changes Associated with Pulmonary Hypertension
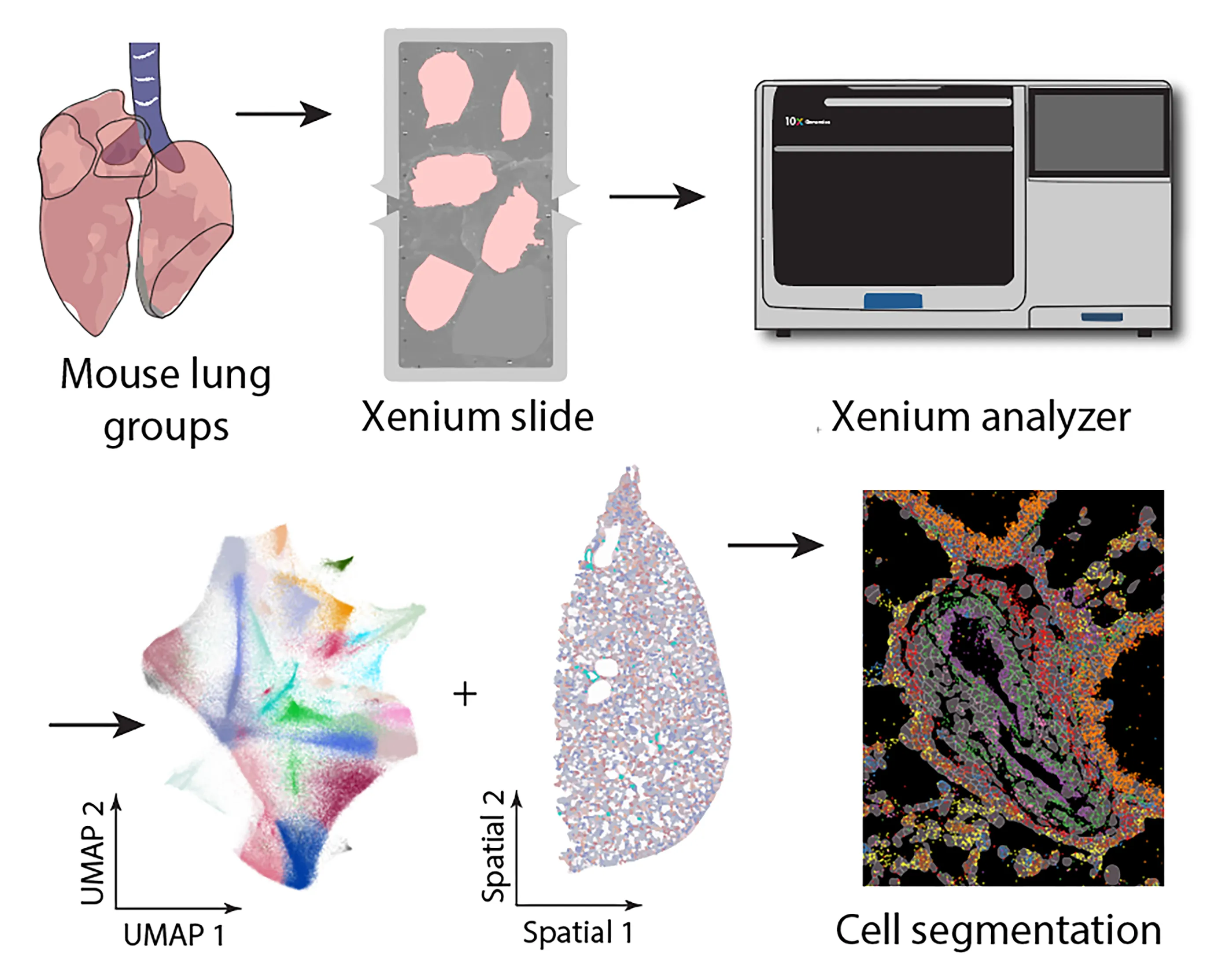
Spatial transcriptomics technologies have emerged as powerful tools for understanding cellular identity and function within the natural spatial context of tissues. Traditional transcriptomics techniques, such as bulk and single-cell RNA sequencing, lose this spatial information, which is critical for addressing many biological questions. Here, we present a protocol for high-resolution spatial transcriptomics using fixed frozen mouse lung sections mounted on 10X Genomics Xenium slides. This method integrates multiplexed fluorescent in situ hybridization (FISH) with high-throughput imaging to reveal the spatial distribution of mRNA molecules in lung tissue sections, allowing detailed analysis of gene expression changes in a mouse model of pulmonary hypertension (PH). We compared two tissue preparation methods, fixed frozen and fresh frozen, for compatibility with the Xenium platform. Our fixed frozen approach, utilizing a free-floating technique to mount thin lung sections onto Xenium slides at room temperature, preserved tissue integrity and maximized the imaging area, resulting in high-fidelity spatial transcriptomics data. Using a predesigned 379-gene mouse panel, we identified 40 major lung cell types. We detected key cellular changes in PH, including an increase in arterial endothelial cells (AECs) and fibroblasts, alongside a reduction in capillary endothelial cells (CAP1 and CAP2). Through differential gene expression analysis, we observed markers of endothelial-to-mesenchymal transition and fibroblast activation in PH lungs. High-resolution spatial mapping further confirmed increased arterialization in the distal microvasculature. These findings underscore the utility of spatial transcriptomics in preserving the native tissue architecture and enhancing our understanding of cellular heterogeneity in disease. Our protocol provides a reliable method for integrating spatial and transcriptomic data using fixed frozen lung tissues, offering significant potential for future studies in complex diseases such as PH.
Open Access
Review
13 January 2025Comparative Analysis of Idiopathic Pulmonary Fibrosis and Progressive Pulmonary Fibrosis: Epidemiology, Pathophysiology, Clinical Features, Diagnosis and Treatment
Idiopathic pulmonary fibrosis (IPF) is a chronic fibrosing interstitial disease of unknown origin, characterized by radiological and histological features consistent with usual interstitial pneumonia (UIP). It is marked by a progressive worsening of dyspnea and a decline in lung function. Both IPF and PPF are comparable because they have poor prognoses with a median survival time from diagnosis of around 2–4 years without antifibrotic therapy. This review shows the main specific characteristics and differences of epidemiology, pathophysiology, clinical and radiological features, treatment, and prognosis of IPF and PPF.
Open Access
Review
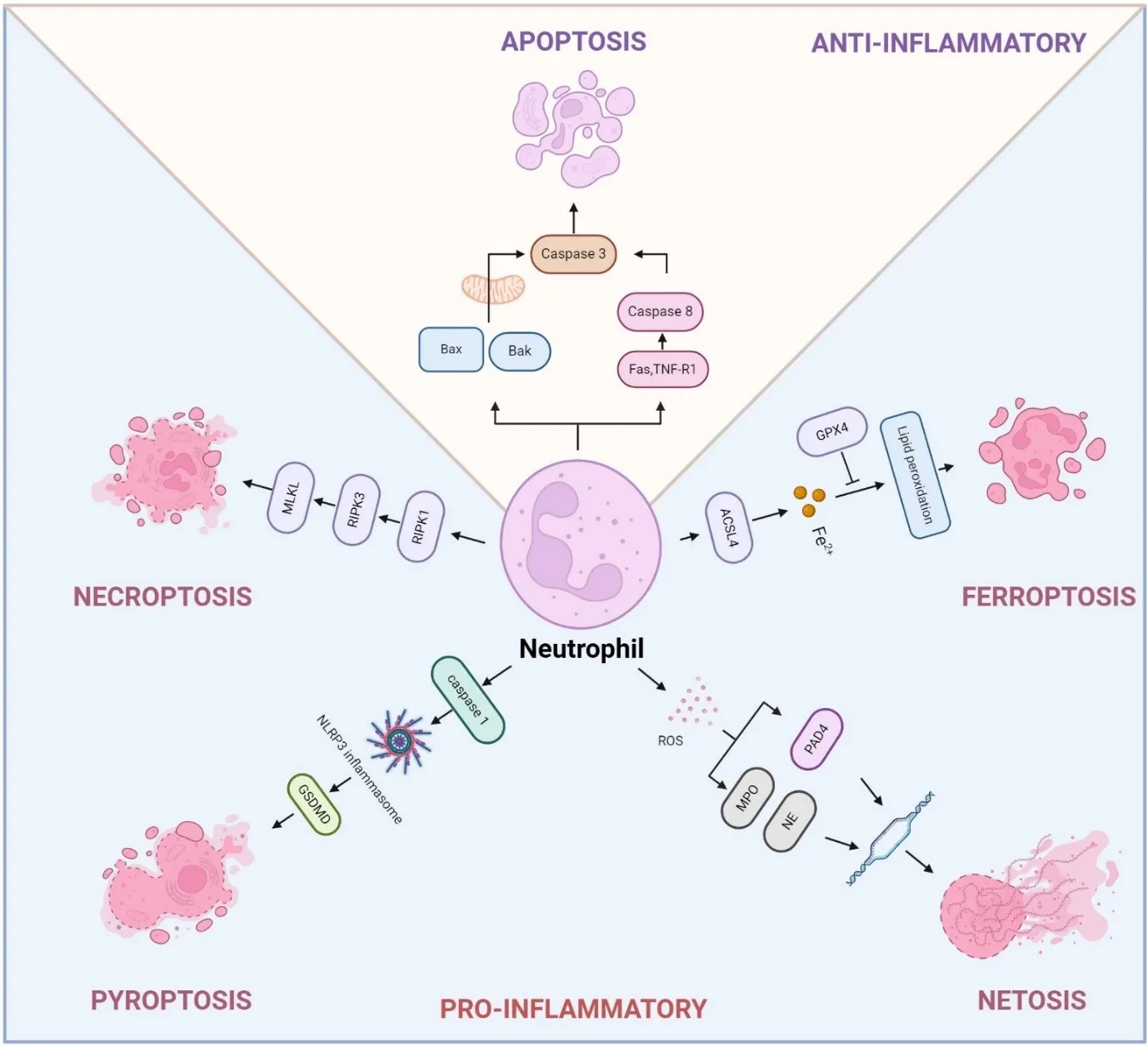
09 December 2024The Multifaceted Roles of Neutrophil Death in COPD and Lung Cancer
Chronic obstructive pulmonary disease (COPD) and lung cancer are closely linked, with individuals suffering from COPD at a significantly higher risk of developing lung cancer. The mechanisms driving this increased risk are multifaceted, involving genomic instability, immune dysregulation, and alterations in the lung environment. Neutrophils, the most abundant myeloid cells in human blood, have emerged as critical regulators of inflammation in both COPD and lung cancer. Despite their short lifespan, neutrophils contribute to disease progression through various forms of programmed cell death, including apoptosis, necroptosis, ferroptosis, pyroptosis, and NETosis, a form of neutrophil death with neutrophil extracellular traps (NETs) formation. These distinct death pathways affect inflammatory responses, tissue remodeling, and disease progression in COPD and lung cancer. This review provides an in-depth exploration of the mechanisms regulating neutrophil death, the interplay between various cell death pathways, and their influence on disease progression. Additionally, we highlight emerging therapeutic approaches aimed at targeting neutrophil death pathways, presenting promising new interventions to enhance treatment outcomes in COPD and lung cancer.
Open Access
Meeting Report
04 December 2024Progress and Gaps in Respiratory Disease Research and Treatment: Highlights of the IRM 2024 in Shanghai
Respiratory diseases pose a major public health challenge globally, necessitating collaborative efforts between basic researchers and clinicians for effective solutions. China, which is heavily impacted by a broad spectrum of respiratory disorders, has made notable strides in both research and clinical management of these diseases. The International Respiratory Medicine (IRM) meeting was organized with the primary goal of facilitating the exchange of recent research developments and promoting collaboration between Chinese and American scientists in both basic and clinical research fields. This article summarizes key insights from IRM2024, held in Shanghai, where a wide range of topics were discussed, including lung tissue development, disease mechanisms, and innovative therapeutic strategies. By integrating perspectives from basic, translational, and clinical research, IRM2024 highlighted recent advancements, addressed persistent challenges, and explored future directions in respiratory science and clinical practice. The insights gained from IRM2024 are poised to be pivotal in shaping future research and therapeutic approaches, further reinforcing the global commitment to enhancing respiratory health and improving patient outcomes.
Open Access
Review
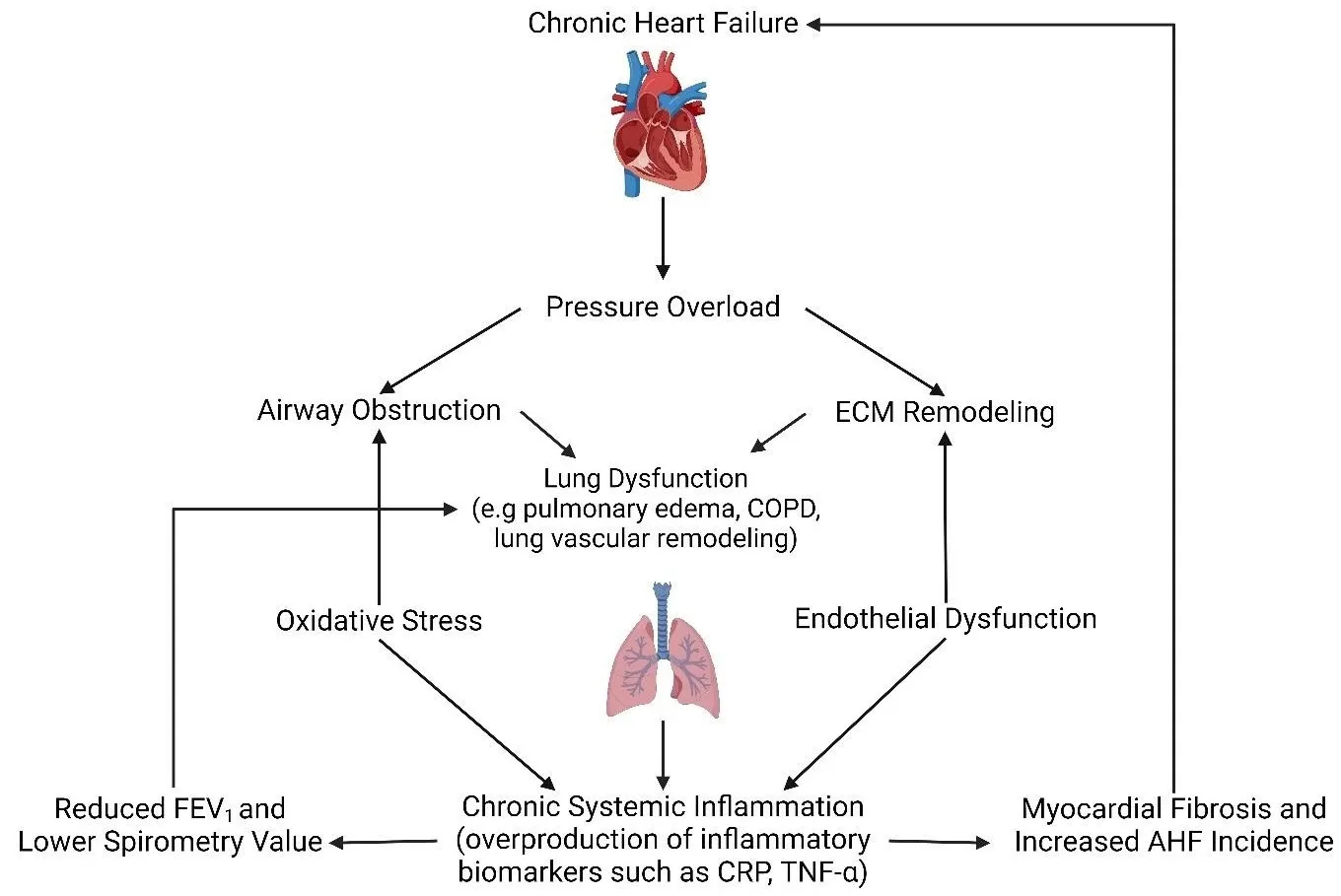
02 December 2024The Interplay of Heart Failure and Lung Disease: Clinical Correlations, Mechanisms, and Therapeutic Implications
Heart failure (HF) is a common clinical syndrome marked by reduced cardiac output, elevated intracardiac pressures, and heart dysfunction. Chronic HF (CHF) is a syndrome characterized by a lack of blood flow and impaired pumping ability to the heart over time, while acute HF (AHF) arises suddenly due to incidents like myocardial infarction or cardiac arrest. HF has a significant impact on pulmonary health and function, leading to conditions such as pulmonary edema and restrictive lung patterns. Clinical evidence highlights the bidirectional relationship between HF and lung dysfunction. Declining lung function serves as a predictor for HF progression and severity, while HF contributes to worsening lung health. Animal models that induce HF through surgical methods further demonstrate the connection between heart and lung pathology. The main mechanisms linking HF and lung dysfunction are pressure overload and chronic systemic inflammation, with changes in the extracellular matrix (ECM) also playing a role. Additionally, environmental factors like air pollution exacerbate lung inflammation, increasing the risk of both HF and chronic obstructive pulmonary disease (COPD) incidence. Combined treatment approaches involving pharmaceutical drugs such as statins, Angiotensin-converting enzyme (ACE) inhibitors, and Angiotensin receptor blockers (ARBs) may benefit by reducing inflammation. This review will explore the complex interplay between HF and lung function, emphasizing their interconnected pathophysiology and potential integrated treatment strategies.
Open Access
Review
15 November 2024Ion Channels in the Immune Response of Asthma
Asthma is a common respiratory disorder characterized by chronic inflammation of the lower airways, contributing to significant morbidity, mortality, and a substantial global economic burden. It is now understood as a heterogeneous condition, with ongoing research shedding light on its complex immunological underpinnings. Ion channels, which are specialized transmembrane proteins that facilitate ion movement based on electrochemical gradients, play a crucial role in the pathophysiology of asthma. Ion channels regulate essential processes like maintaining epithelial hydroelectrolyte balance and also play a role in modulating immune responses involved in asthma. We discuss the connection between ion channel activity and immune regulation in asthma, focusing on ion channel regulation of immune cell behavior, airway hyperresponsiveness, and inflammation in asthma. Understanding ion channels in asthma could lead to the development of targeted therapies modulating their activity, thereby enhancing disease management and patient outcomes.
Open Access
Review
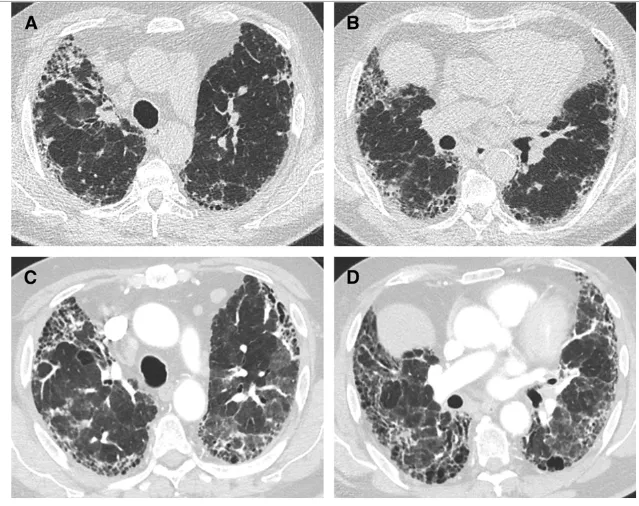
28 October 2024Acute Exacerbations of Interstitial Lung Disease: Evolving Perspectives on Diagnosis and Management
Interstitial lung diseases (ILDs) are a heterogeneous group of chronic lung diseases caused by several potential etiologies but for many, the cause of a given ILD remains unknown. Accurate epidemiologic data are hard to find because of varying definitions, overlapping characteristics once thought to be unique to specific diseases, and ongoing changes in how ILDs are diagnosed and managed. In addition, there are significant variations in prevalence among different geographic populations, likely reflecting a combination of genetic and environmental differences. Certain risk factors, including exposure to cigarette smoke or environmental toxicants (asbestos, silica, fracking, coal dust, and air pollution), genetic mutations, and single nucleotide polymorphisms, have all been associated with developing interstitial lung disease. Due to the availability of high-resolution computed tomography (CT) scans, earlier and broader recognition of subtle imaging changes, and an aging worldwide population, the incidence and prevalence of ILDs are increasing. While a given cause of particular interstitial lung disease may vary, patients often experience breathlessness and a non-productive cough due to impaired alveolar gas exchange. Patients with ILD are prone to the development of acute exacerbations, marked by acute or chronic respiratory failure because of an acute exacerbation of the underlying lung disease. In this review, we discuss the definition of an acute exacerbation and comment on what is known about the underlying pathophysiology in exacerbations of idiopathic pulmonary fibrosis and other ILDs. We also emphasize the similarities in the clinical presentation of the acute exacerbations regardless of the underlying ILD, highlight key prognostic features of the diagnosis, and underscore the importance of interdisciplinary management of acute interstitial lung disease exacerbations.
Open Access
Commentary
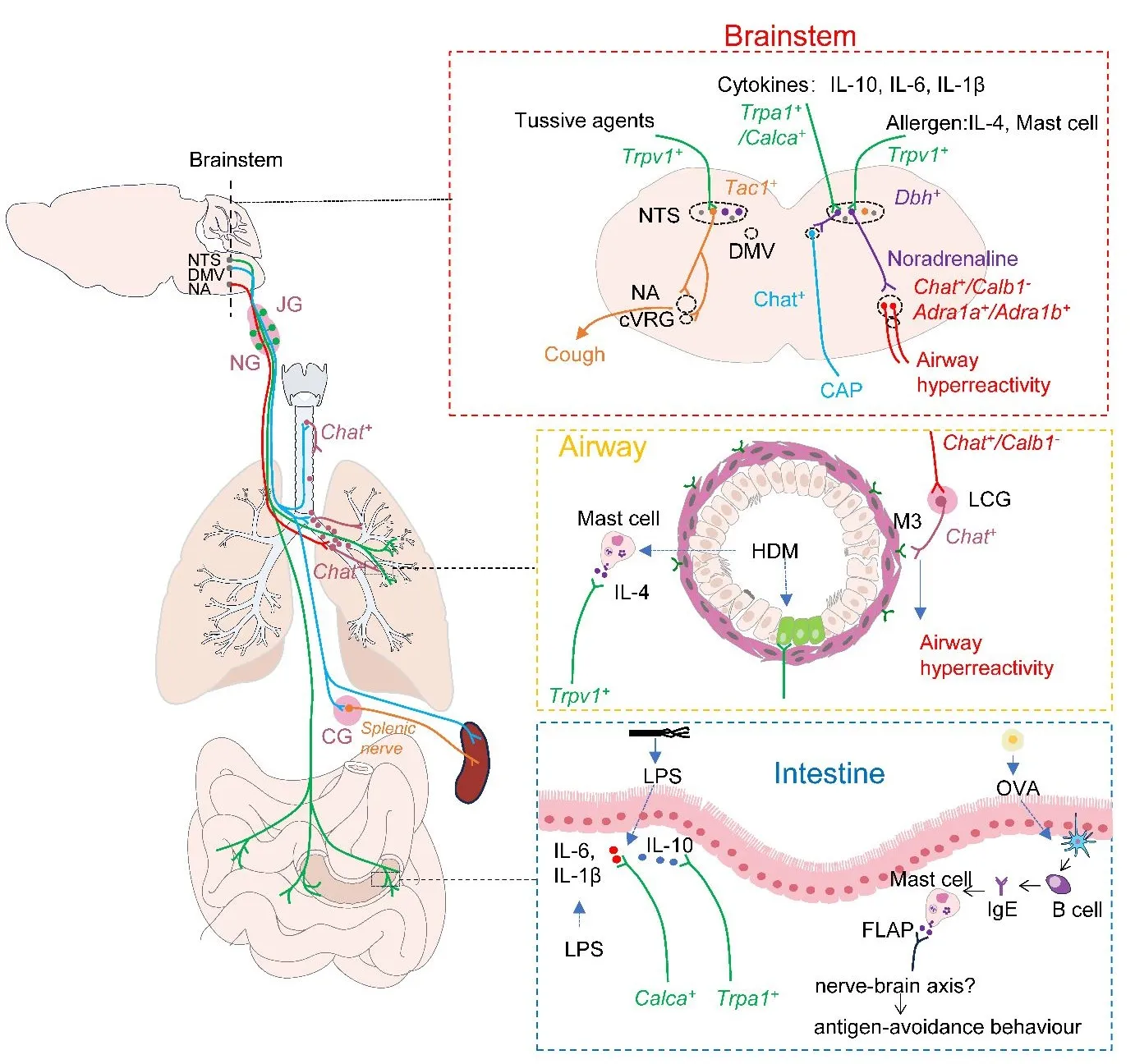
18 September 2024Primed Lung−Vagus−Brainstem Circuit by Allergen Triggers Airway Hyperactivity
The nucleus of the solitary tract (NTS) is the primary hub for sensing and integrating respiratory information. It integrates input from the vagus and glossopharyngeal nerve. It interacts with other brainstem nuclei, such as the nucleus ambiguus (NA) and the dorsal motor nucleus of the vagus (DMV), to transmit information and initiate a neuroreflex response to respiratory stimuli. In a recent issue of the journal Nature, Su et al. demonstrated that Dbh+ neurons in the NTS can receive signals from vagal Trpv1+ sensory neurons that sense allergen−induced IL−4 production in mast cells and pass the signal to Chat+ neurons in the NA by releasing norepinephrine. Subsequently, NA Chat+ neurons drive allergen−induced airway hyperresponsiveness by projecting onto cholinergic pulmonary ganglia in the lungs. This study not only provides new insights into the regulation of allergen−induced airway hyperresponsiveness by lung−vagus–brainstem interoceptive circuit but also provides us with new strategies to combat asthma.